The ‘Mistakes and Mishaps in Healthcare’ Movement
| Home | | Pharmacovigilance |Chapter: Pharmacovigilance: Teaching and Learning Pharmacovigilance
Well-publicized studies of mistakes and mishaps in care of hospitalized patients in both the United States (Brennan et al., 1991) and Australia (Wilson et al., 1995) led to substantially heightened levels of public interest in achieving less harm from customarily delivered health care.
THE ‘MISTAKES AND MISHAPS IN
HEALTHCARE’ MOVEMENT
Well-publicized
studies of mistakes and mishaps in care of hospitalized patients in both the
United States (Brennan et al., 1991)
and Australia (Wilson et al., 1995)
led to substantially heightened levels of public interest in achieving less
harm from customarily delivered health care. In the United States, a landmark
Institute of Medicine report To err is
human (Kohn et al., 2000) acted
as a platform to launch a range of initiatives
to draw attention to and improve patient safety.
Parallel
action was taken in the United Kingdom and other countries to address rising
public concern about the high levels of patient injury and morbid-ity occurring
because of patient contact with estab-lished healthcare systems. In the United
Kingdom, a pivotal report from the NHS chief medical offi-cer (Donaldson, 2000)
led to the establishment of a National Patient Safety Agency that was tasked
with reporting, analysing and disseminating the lessons of adverse events and
‘near misses’ involving British NHS patients.
Embedded
within reports associated with this move-ment are the documentation of
significant numbers of incidents associated with medication use, and by
implication, unsafe healthcare practice. Recently, in the United Kingdom, 9% of
reported patient safety incidents in acute hospitals and 21% of such incidents in
general practice were noted to be associated with medications (Scobie et al., 2005). The relationship between
medication errors and adverse drug events is complex, with medication errors
being generally more common than adverse drug events. It has been estimated
that about a third to a half of adverse drug events are typically associated
with medication errors: however, of course, not all adverse drug events
necessarily spring from medication errors (Morimoto et al., 2004).
The
close intersection of medication error and adverse drug events now demands
careful attention in curricula associated with pharmacovigilance. Whilst the
generally accepted definition of medication error asserts that by their nature,
such errors must be preventable (National Coordinating Council for Medi-cation
Error Reporting and Prevention, 1995), and other respected workers in the field
have suggested that medication errors might also be ‘ameliorable’: a kind of
gradation of preventability (Morimoto et
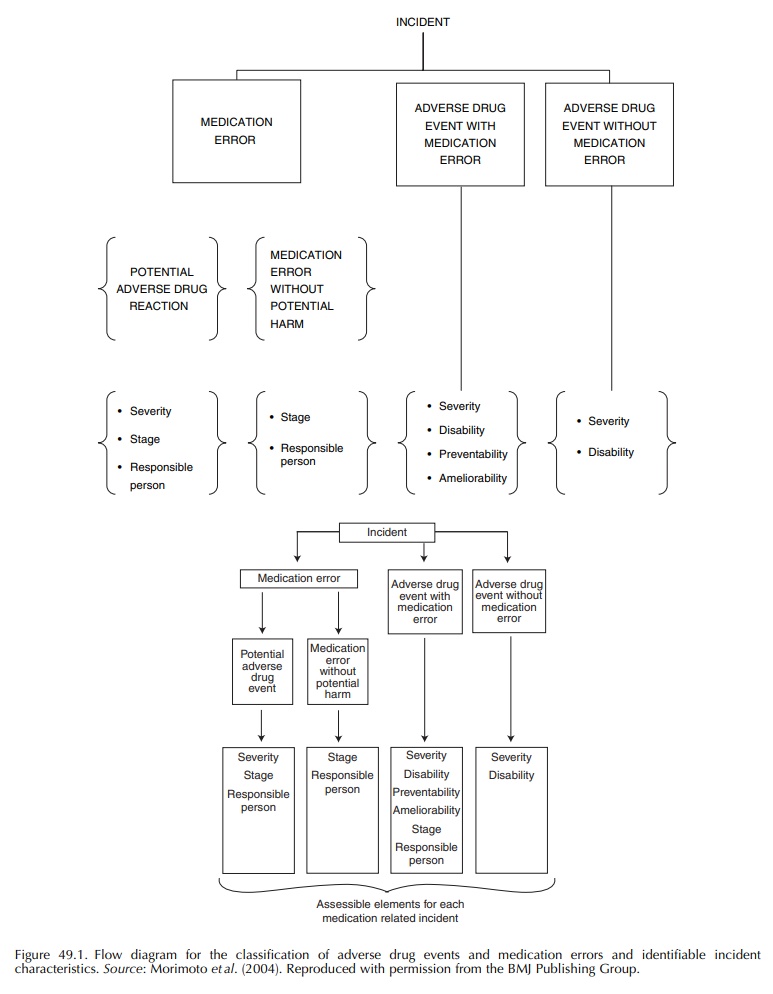
al., 2004). Morimoto and colleagues propose a comprehensive system for detecting and classifying
medication-related incidents and suggest that in rela-tion to each such
incident, gaugings can be taken of the level of severity, resultant disability,
preventabil-ity or ameliorability as well as the stage and setting of care when
such incidents occur (Figure 49.1).
There are clearly important implications for use of the term ‘error’ when applied to medication use. As an absolute term, the implication that such inci-dents must be preventable defies the logic of what is known about pharmacotherapy. When does a side effect of a drug become an adverse event, an ADR or a medication-related error? Clearly different players in the healthcare system will have different perceptions on this point.
For
the patient (or the pharmacovigilist notic-ing events recorded in a healthcare
database), what appears to be an error may well prove to have been a conscious
judgement of perceived relative benefit and risk on the part of an individual
prescriber.
‘Error’
may have occurred in such circumstances solely insofar as the decision to use a
drug was not openly shared between prescriber and patient, with both parties
being properly informed about potential benefits and risks associated with
treatment. For the pharmacovigilist, whether an ‘error’ actually occurred often
remains uncertain, depending on the distance in time and space from the event
and its specific circumstances.
Related Topics
