Other β Blockers
| Home | | Pharmacology |Chapter: Essential pharmacology : Antiadrenergic Drugs (Adrenergic Receptor Antagonists) And Drugs For Glaucoma
A number of β blockers have been developed having some special features. The associated properties with their significance can be summarized as:
OTHER β BLOCKERS
A number of β blockers have been
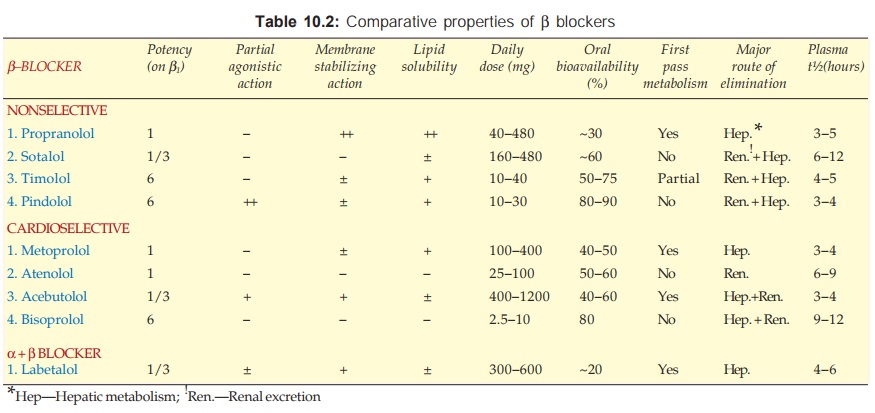
developed having some special features. Their comparative properties are
presented in Table 10.2. The associated properties with their significance can
be summarized as:
Cardioselectivity (in metoprolol,
atenolol, acebutolol, bisoprolol, nebivolol).
These drugs are more
potent in blocking cardiac (β1) than bronchial (β2) receptors. However,
selectivity is only relative and is lost at high doses. Their features are:
·
Lower propensity to cause bronchoconstriction,
but even these drugs should be avoided, if possible, in asthmatics.
·
Less interference with carbohydrate metabolism
and less inhibition of glycogenolysis during hypoglycaemia—safer in diabetics. However,
tachycardia in response to hypoglycaemia is blocked.
·
Lower incidence of cold hands and feet, less chances
of precipitating Raynaud’s phenomenon.
·
No/less deleterious effect on blood lipid
profile.
·
Ineffective in suppressing essential tremor
(it occurs through β2 action on muscle
fibres).
·
Less liable to impair exercise capacity.
Partial Agonistic (Intrinsic Sympathomimetic) Action (in pindolol,
acebutolol). These drugs themselves activate β1 and/or β2 receptors
submaximally. The benefits of this property are controversial.
·
Bradycardia and depression of contractility at
rest are not prominent, but exercise tachycardia is blocked; may be preferred
in those prone to severe bradycardia (elderly patients; sick sinus) or with low
cardiac reserve.
·
Withdrawal is less likely to exacerbate hypertension
or angina; continued agonistic action on receptors (of the drug itself)
prevents development of supersensitivity.
·
Plasma lipid profile is not/less worsened.
·
Not effective in migraine prophylaxis—they
dilate cerebral vessels.
·
Not suitable for secondary prophylaxis of MI.
Membrane Stabilizing
Activity (in propranolol, oxprenolol,
acebutolol). This activity is claimed to contribute to the antiarrhythmic
action, but appears to be significant only at high doses.
Lipid Insolubility (atenolol, sotalol)
·
They are less likely to produce central
effects.
·
They are incompletely absorbed orally, but do
not undergo first pass metabolism and are primarily excreted unchanged in
urine: are longer acting (t½ 6–20 hours) and tend to be effective in a narrow
dose range. In contrast, the lipid soluble agents are primarily metabolized in
liver and have shorter t½ (2–6 hours).
Salient
features of important β blockers are given below.
1. Sotalol Nonselective β blocker with lower lipid solubility. It has additional K+ channel
blocking and class III antiarrhythmic property.
SOTAGARD
40, 80 mg tab.
2. Timolol It is the β blocker preferred for topical use in eye (see p. 144).
Orally
it is a potent β blocker—has been used in hypertension, angina and prophylaxis
of myocardial infarction.
Betaxolol, Levobunolol, Cartiolol and Metipranolol are β blockers employed exclusively for topical application to the eye
(see p. 145).
3. Pindolol A potent β blocker with prominent intrinsic sympathomimetic activity. It has
been used primarily as antihypertensive: may be advantageous in patients who
develop marked bradycardia with propranolol. Chances of rebound hypertension on
withdrawal are also less. The effective dose range is rather narrow.
PINADOL 5 mg tab, VISKEN
10, 15 mg tab.
4. Metoprolol It is the prototype of
cardioselective (β1) blockers; nearly 50
times higher dose is needed to block isoprenaline induced vasodilatation. It is
less likely to worsen asthma, but is not entirely safe. It may be preferred in
diabetics receiving insulin or oral hypoglycaemics. Patients who complain of
cold hands and feet while on propranolol do better on metoprolol.
First
pass metabolism of metoprolol is less marked than propranolol, but 90% or more
is ultimately metabolized before excretion. There are slow and fast
hydroxylators of metoprolol (CYP2D6 alleles); the former may require a lower
dose.
Side
effects of metoprolol are milder. It is generally given orally, but i.v.
injection (5–15 mg) has been used in myocardial infarction provided bradycardia
is absent.
BETALOC
25, 50, 100 mg tab, 5 mg/ml inj. LOPRESOR, METOLAR 50, 100 mg tab.
S(–) Metoprolol is the active
enantiomer, now available as a single
enantiomer product. It is to be used at half the dose as the recemate.
Dose: 12.5–50 mg OD–BD.
METPUREXL 12.5, 25, 50
mg extended release tabs.
5. Atenolol A relatively selective β1 blocker having low lipid solubility. It is
incompletely absorbed orally, but first pass metabolism is not significant.
Because of longer duration of action, once daily dose is often sufficient. Side
effects related to CNS action are less likely. No deleterious effects on lipid
profile have been noted. Effective dose for most individuals falls in a narrow
range. It is one of the most commonly used β blockers for
hypertension and angina.
BETACARD, ATEN,
TENORMIN 25, 50, 100 mg tab.
S(–) Atenolol This pure active
enantiomer is effective at half the
dose and may be better tolerated.
Dose: 12.5–50 mg OD;
ATPURE 12.5, 25, 50 mg
tabs.
6. Acebutolol Another
cardioselective agent with significant
partial agonistic and membrane stabilizing properties. Effect on resting heart
rate is less. The side effect profile is like that of metoprolol. Acebutolol is
rapidly metabolized to an active metabolite diacetolol which is primarily
excreted by kidney and has a longer t½ (8–12 hours). As such, a single daily
dose is sufficient in many patients.
SECTRAL 200, 400 mg tab., 10 mg/2 ml amp.
Intravenous dose for
arrhythmias 20–40 mg.
7. Bisoprolol A cardioselective β blocker lacking
intrinsic sympathomimetic activity; suitable for once daily administration in
angina, hypertension and CHF.
CONCOR, CORBIS 5 mg
tab; ½ to 2 tab OD.
8. Esmolol It is an ultrashort
acting β1 blocker devoid of partial
agonistic or membrane stabilizing actions. It is inactivated by esterases in
blood; plasma t½ is < 10 min; action disappears 15–20 min after terminating
i.v. infusion—degree of β blockade can be titrated by regulating rate
of infusion. Rapid onset, short lasting fall in BP attends i.v. infusion of
esmolol.
A loading dose of 0.5
mg/kg is given followed by 0.05–0.2 mg/kg/min infusion. It has been used to
terminate supraventricular tachycardia, episodic atrial fibrillation or
flutter, arrhythmia during anaesthesia, to reduce HR and BP during and after
cardiac surgery, and in early treatment of myocardial infarction.
MINIBLOCK 100 mg/10 ml,
250 mg/10 ml inj.
9. Celiprolol It is a selective β1 blocker having additional weak β2 agonistic activity
which reduces vascular resistance and holds promise of safety in asthmatics.
Nonadrenoceptor media ted vasodilatation (probably due to NO production) adds
to its antihypertensive action.
Dose: 200–600 mg OD; CELIPRES 100, 200 mg tab.
10. Nebivolol
This highly selective β1 blocker also acts as a NO
donor, produces vasodilatation and has the potential to improve endothelial
function, which may delay atherosclerosis. In contrast to older β blockers, hypotensive
response to nebivolol has a rapid onset. It has been used in hypertension and
CHF.
Dose: 5 mg (elderly 2.5 mg)
OD;
NEBICARD 2.5, 5 mg
tabs, NODON 5 mg tab.
Related Topics
