The Process of Regulatory Pharmacovigilance in the EU
| Home | | Pharmacovigilance |Chapter: Pharmacovigilance: Regulatory Pharmacovigilance in the EU
Regulatory pharmacovigilance is dependent on the availability of information on the clinical effects of medicines in representative populations as used in normal practice.
THE PROCESS OF REGULATORY
PHARMACOVIGILANCE IN THE EU
Regulatory
pharmacovigilance is dependent on the availability of information on the
clinical effects of medicines in representative populations as used in normal
practice. In addition to systems for collect-ing and handling suspected ADRs,
processes for iden-tifying and investigating signals are necessary. All
potentially important hazards are investigated with a view to taking
appropriate action based on the avail-able scientific evidence. The most
important outputs of the process are actions to promote safer use of medicines.
These include, for example introducing warnings, contraindications, information
on ADRs or changes to dosing recommendations. Indications or methods of supply
may also be restricted, although withdrawal of a medicinal product from the
market on safety grounds is relatively unusual (Jefferys et al., 1998). Informing users and explaining the reasons for the
action taken is a critical determinant of the effec-tiveness of these measures.
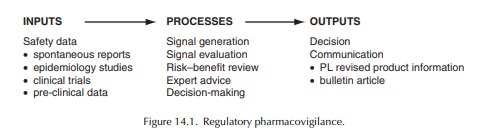
The process of regulatory pharmacovigilance is summarised in Figure 14.1.
RISK MANAGEMENT
With
a view to increase proactivity, the recently revised legislation has introduced
the concept of risk management which is defined in the EU as a set of
pharmacovigilance activities and interventions designed to identify,
characterise, prevent or minimise risks relating to medicinal products,
including the assessment of the effectiveness of those interventions. Some of
its elements have already been agreed by the ICH in guideline E2E on
pharmacovigilance planning and, together with current thinking, incorporate a
‘best evidence’ approach of the excellence model in pharma-covigilance (Waller
and Evans, 2003). In terms of risk management, there is a need for use of best
expertise and methods in safety studies and epidemiology to take this forward.
DETECTION OF ADRs
Potentially
important safety issues can be identi-fied at any stage of drug development. In
the post-authorisation phase, they are particularly likely to be identified in
the first few years after marketing, although new issues also arise with
long-established medicines. To ensure that safety problems which have not been
recognised or fully understood pre-marketing are handled promptly, proactive
processes are used for screening emerging data for potential issues and
bring-ing together all the available information from multiple sources. In
regulatory practice, a signal is an alert from any available source that a
medicine may be associated with a previously unrecognised hazard or that a
known hazard may be quantitatively (e.g. more frequent) or qualitatively (e.g.
more serious) different from existing expectations.
The
commonest source for identification of signifi-cant safety concerns arising
with marketed medicines is spontaneous ADR reporting. These are individual case
reports from health professionals of adverse events which the reporter
considers may be related to the medicine(s) being taken. Reporters are not
asked to provide all adverse events that follow administration of the medicine
but to selectively report those which they suspect were ADRs. There is
frequently confu-sion between the terms ‘adverse event’ and ‘adverse reaction’
which can be avoided by using the term ‘suspected
adverse reaction’ when referring to a case or series of cases reported through
a spontaneous report-ing scheme. The term ‘adverse event’ should be used in the
context of studies where all events are being collected regardless of whether
or not they are suspected to be related to a drug. This approach is underpinned
by standard definitions given in EU legislation (Title I of Directive
2001/83/EC) and is also consistent with definitions proposed by the ICH in
guidelines E2A and E2D (International Conference on Harmonisation, 2005).
Although
formal studies of drug safety are partic-ularly used in the investigation of
signals identi-fied by methods such as spontaneous ADR report-ing (i.e.
hypothesis-testing), they may also provide the initial evidence producing a
safety concern. Signals may also be detected from other sources such as
literature reports and from screening of the international spon-taneous
reporting database operated by the Uppsala Monitoring Centre in Sweden, a
Collaborating Centre of the World Health Organization (Uppsala Monitoring
Centre, 2005) to which EU Member States contribute data. Whatever the source of
the signal, the aim is to identify it as rapidly as possible. The next steps
are to inform other Member States, gather further information and conduct an
evaluation.
EVALUATION OF PHARMACOVIGILANCE ISSUES
When
there is sufficient evidence of a hazard to warrant further investigation,
detailed consideration is given to causality, possible mechanisms, frequency
and preventability. Assessment of these issues may require new epidemiological
studies, but the hypothesis may be strengthened or weakened using immediately
available sources of retrospective information such as worldwide spontaneous
reporting, published literature and epidemiological databases.
The
broad principles relating to post-authorisation studies have been set out in
guidelines for marketing authorisation holders (European Commission, 2006).
When new data become available from purpose-designed studies, it is important
that they are reviewed in the context of the existing data. An assessment is
made of whether and how the new evidence changes the previ-ous evaluation,
focusing particularly on the strength of the evidence for a drug-related
association and possible approaches to prevention. In the latter respect,
detailed analysis of the data to identify possible risk factors for the hazard
is important.
The
output of an evaluation is an assessment report that brings together the key
information on the hazards and facilitates discussion of the risks and benefits
of the medicine and possible measures which may facil-itate safe use. Experts
in pharmacoepidemiology and relevant therapeutic areas are consulted and
involved in such discussions both at national and EU level.
DECISION-MAKING
The
objective of the EU competent authorities is to take regulatory actions which
are justified by scien-tific evidence and allow users to make informed
deci-sions and to use medicines safely. Sometimes, the balance of risks and
benefits will be sufficiently clear to allow firm recommendations (such as
contraindica-tions), whereas in other situations less directive advice will be
warranted.
The
types of action which may be taken vary accord-ing to potential means of
preventing the ADR. In particular, hazards may be minimised by targeting the
medicine at patients least likely to be at risk of the ADR and by specifically
contraindicating it in patients with identifiable risk factors. Dose and
duration of treatment are often important issues as the risk of many hazards is
related to one or both of these parameters. It is quite common for dosage
regimens to change during the post-marketing period in response to safety
concerns, and many medicines have been initially recommended at doses higher
than necessary. In re-evaluating dose in response to a safety concern,
consideration is also given to the evidence of efficacy at lower doses.
The
identification of a new ADR or the accumulation of important new evidence about
a recognised reaction leads to a need to make changes to the product
infor-mation and hence to vary the marketing authorisa-tion(s). Variations to marketing
authorisations on safety grounds may be proposed by the competent author-ity or
the pharmaceutical company. Regardless of who proposes the changes, there is
exchange of informa-tion and discussion between the parties before a vari-ation
is submitted to facilitate rapid implementation. When the competent authorities
and companies are in agreement about the nature and impact of a drug safety
issue, changes can be made on a voluntary basis by the marketing authorisation
holder. However, if companies do not agree about the actions required, then the
competent authorities may exercise compul-sory powers. In situations of
particular urgency, the legislation provides for rapid processing of safety
vari-ations where either the marketing authorisation holder or the competent
authority can initiate an urgent safety restriction (USR) procedure that
enables a change to the product information within 24 hours and is followed
within 2 weeks by a formal variation (Commission Regulation (EC) No. 1084/2003;
Commission Regu-lation (EC) No. 1085/2003). Exceptionally, when the issue has
urgent public health implications, the author-ities may immediately withdraw
the product(s) from the market. This can be effected either by suspen-sion of
the authorisation(s) or by its revocation. The option to suspend is considered
in situations whereby an urgent temporary measure is required as a precau-tion
to protect public health whilst awaiting new data to emerge. Revocation is
foreseen when data are already available demonstrating an unfavourable
benefit–risk balance even in different sub-groups of patients.
COMMUNICATION
Communicating
information to users of medicinal prod-ucts is a vital step in the process of
handling a safety issue with a marketed medicine. An important consideration is
how quickly information needs to be made available to users. A new
life-threatening ADR requires imme-diate communication, whereas the addition of
informa-tion relating to a non-serious ADR could be added at the next routine
revision of the product information. The distribution of safety information may
be targeted at specialists or generalists or both, other relevant health
professionals and at patients. The recently revised legis-lation has introduced
new obligations for the Member States’ authorities and the EMEA in relation to
such communication to the public. Additional requirements are also imposed on
the companies and will even be enforced by penalty legislation. A particularly
impor-tant aim in communications about drug safety is to ensure that essential
information is clearly conveyed and not obscured by other less important
information. Every effort is therefore made to word the key facts and
recommendations unambiguously.
The
key principles with patient information are that it should, in substance, be
the same as the informa-tion provided to health professionals and it should be
presented in language that the patient can understand. Good patient information
adds to and reinforces the main issues that should be discussed between health
professionals and patients and does not make state-ments which could interfere
with that relationship. To respond appropriately to the patients’ demands, an
EMEA/CHMP Working Group with Patient Organisa-tions is in operation since 2003
with one of its aims to provide overall recommendations and specific input to
guidelines on communication and to new proce-dures, for example for testing of
product information (EMEA/CHMP Working Group with Patient Organisa-tions,
2005). Similar initiatives have been undertaken at national level in some
Member States and there is fruitful exchange of all experience gained.
Any
change to the marketing authorisation and prod-uct information which has
significant safety implica-tions is actively drawn to the attention of the
rele-vant health professionals, usually by circulating the new product
information under cover of a ‘Dear Doctor/Pharmacist’ letter (Direct Healthcare
Profes-sional Communication). With regard to information targeted at health
professionals, the EMEA has initi-ate dialogue with health professional
organisations at EU level to support and complement national activities. When
the changes being made are vital for ensuring patient safety, they are
implemented very quickly, and it is normal practice to make information available
to the media and general public through press releases and/or the Internet.
Improvements in dissemination mecha-nisms are planned for the future.
The
competent authorities recognise that successful communication about drug safety
is a vital component of the pharmacovigilance process and needs EU-wide
co-ordination. This is a particular challenge because of the need to translate
messages into all the official languages used in the EU (currently 20), and
consid-erable attention is being paid to improving this aspect of the process.
Intensive thought is currently given to the enforcement of existing and
establishment of new procedures to optimise EU-wide co-ordination of safety
communication as well as to the assessment of public health impact of such
communication. In terms of risk minimisation, targeted information to
healthcare professionals and patients is seen as an important tool.
Related Topics
