Antiparkinsonian Drugs
| Home | | Pharmacology |Chapter: Essential pharmacology : Antiparkinsonian Drugs
These are drugs that have a therapeutic effect in parkinsonism.
ANTIPARKINSONIAN
DRUGS
These are drugs that have a therapeutic effect in parkinsonism.
Belladonna alkaloids had been empirically
used in PD. A breakthrough was made
in 1967 when levodopa was found to
produce dramatic improvement. Its use
was based on sound scientific investigations made in the preceding 10 years
that—DA is present in the brain; it (along with other monoamines) is depleted
by reserpine; reserpine induced motor defect is reversed by DOPA (the precursor
of DA); striatum of patients dying of PD was deficient in DA. Thus, parkinsonism
was characterized as a DA deficiency state and levodopa was used to make good
this deficiency, because DA itself does not cross the bloodbrain barrier. In
the subsequent years, a number of levodopa potentiators and DA agonists have
been developed as adjuvants/ alternatives.
Classification
1. Drugs affecting brain
dopaminergic system
a.
Dopamine Precursor : Levodopa (ldopa)
b.
Peripheral Decarboxylase
Inhibitors : Carbidopa,
Benserazide.
c.
Dopaminergic Agonists: Bromocriptine, Ropinirole, Pramipexole
d.
MAO-B Inhibitor: Selegiline
e.
COMT Inhibitors: Entacapone,
Tolcapone
f.
Dopamine Facilitator: Amantadine.
2. Drugs affecting brain
cholinergic system
a. Central Anticholinergics: Trihexyphenidyl (Benzhexol), Procyclidine, Biperiden.
b. Antihistaminics : Orphenadrine, Promethazine.
LEVODOPA
Levodopa has a specific salutary effect in PD: efficacy
exceeding that of any other drug used alone. It is inactive by itself, but is
the immediate precursor of the transmitter DA. More than 95% of an oral dose is
decarboxylated in the peripheral tissues (mainly gut and liver). DA thus formed
acts on heart, blood vessels, other peripheral organs and on CTZ (though
located in the brain, i.e. floor of IV ventricle, it is not bound by blood-brain
barrier). About 1–2% of administered levodopa crosses to the brain, is taken up
by the surviving dopaminergic neurones, converted to DA which is stored and
released as a transmitter. Brains of parkinsonian patients treated with levodopa
till death had DA levels higher than those not so treated. Further, those
patients who had responded well had higher DA levels than those who had
responded poorly.
Actions
1. CNS
Levodopa hardly produces any effect in normal individuals
or in patients with other neurological diseases. Marked symptomatic improvement
occurs in parkinsonian patients. Hypokinesia and rigidity resolve first, later
tremor as well. Secondary symptoms of posture, gait, handwriting, speech,
facial expression, mood, self care and interest in life are gradually
normalized.
The effect of levodopa on behaviour has been described as a
‘general alerting response’. In some patients this progresses to excitement—
frank psychosis may occur. Embarrassingly disproportionate increase in sexual
activity has also been noted. Dementia, if present, does not improve; rather it
predisposes to emergence of psychiatric symptoms.
Levodopa has been used to produce a nonspecific ‘awakening’
effect in hepatic coma.
Two subtypes of DA receptors (D1, D2) were originally described.
Three more (D3, D4, D5) have now been identified and cloned. All are G protein
coupled receptors and are grouped into two families:
D1 like (D1, D5) Are excitatory: act by
increasing cAMP formation and PIP2
hydrolysis thereby mobilizing intracellular Ca2+ and activating protein kinase
C through IP3 and DAG.
D2 like (D2, D3, D4) Are inhibitory: act by
inhibiting adenylyl
cyclase/opening K+ channels/depressing voltage sensitive Ca2+ channels.
The various subtypes of DA receptors are differentially
expressed in different areas of the brain, and appear to play distinct roles.
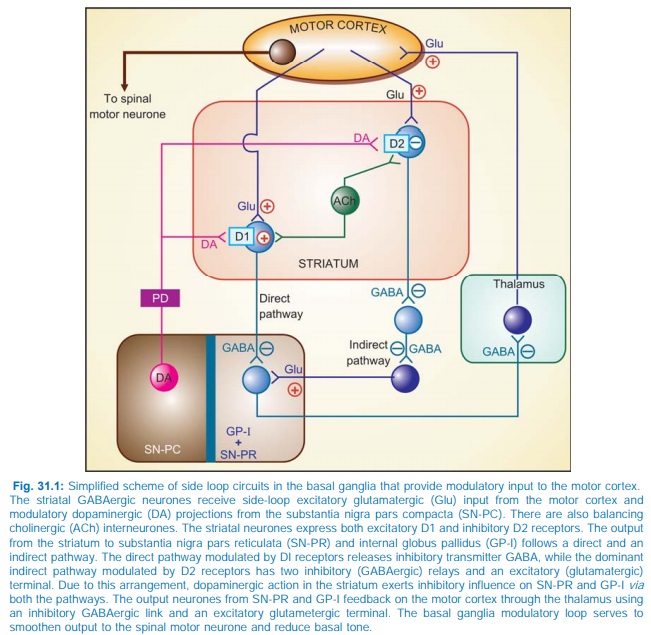
Both D1 and D2 receptors are present in the striatum and are involved in the
therapeutic response to levodopa. They respectively regulate the activity of
two pathways having opposite effects on the thalamic input to the motor cortex
(Fig. 31.1). Thus, stimulation of excitatory D1 as well as inhibitory D2
receptors in the striatum achieves the same net effect of smoothening movements
and reducing muscle tone.
Dopamine receptor in SNPC and in pituitary is also of D2 type.
The D3 receptors predominate in nucleus accumbans and hypothalamus, but are
sparse in caudate and putamen, while D4 and D5 are mostly distributed in neocortex,
midbrain, medulla and hippocampus.
2. CVS
The peripherally formed DA can cause tachycardia by acting
on β adrenergic receptors. Though DA can stimulate vascular adrenergic
receptors as well, rise in BP is not seen. Instead, postural hypotension is
quite common. This may be a central action—DA and NA formed in the brain decrease
sympathetic outflow; also DA formed in autonomic ganglia can impede ganglionic
transmission.
Gradual tolerance develops to both cardiac stimulant and hypotensive
actions.
3. CTZ
Dopaminergic receptors are present in this area and DA acts as an excitatory transmitter. The DA formed peripherally gains access to the CTZ without hindrance—elicits nausea
4. Endocrine
DA acts on pituitary
mammotropes to inhibit prolactin release and on somatotropes to increase GH
release. Though prolactin levels in blood fall during levodopa therapy,
increased GH levels are not noted in parkinsonian patients. Probably the
mechanisms regulating GH secretion are altered in these patients.
Pharmacokinetics
Levodopa is rapidly
absorbed from the small intestines by utilizing the active transport process
meant for aromatic amino acids. Bioavailability of levodopa is affected by:
1. Gastric emptying: if
slow, levodopa is exposed to degrading enzymes present in gut wall and liver
for a longer time—less is available to penetrate bloodbrain barrier.
2. Amino acids present in
food compete for the same carrier for absorption: blood levels are lower when
taken with meals.
Levodopa undergoes high
first pass metabolism in g.i. mucosa and liver. The peripheral and central
pathway of metabolism of levodopa is depicted in Fig. 31.2.
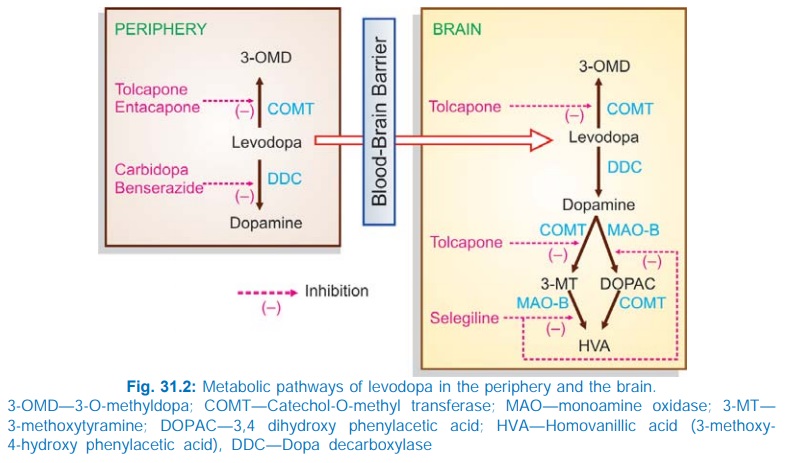
About 1% of administered levodopa that enters brain, aided by
amino acid carrier mediated active transport across brain capillaries, also
undergoes the same transformation. The plasma t½ of levodopa is 1–2 hours.
Pyridoxal is a cofactor for the enzyme dopa-decarboxylase. The metabolites are
excreted in urine mostly after conjugation.
Adverse Effects
Side effects of levodopa therapy are frequent and often
troublesome. Most are dose-related and limit the dose that can be administered,
but are usually reversible. Some are prominent in the beginning of therapy
while others appear late.
At The Initiation Of Therapy
These can be minimized by starting with a low dose.
1. Nausea And Vomiting It occurs in almost every patient. Tolerance gradually develops
and then the dose can be progressively increased.
2. Postural Hypotension It occurs in about
1/3 of patients, but is mostly asymptomatic; some patients experience
dizziness, few have fainting attacks; more common in patients receiving antihypertensives.
Tolerance develops with continued treatment and BP normalizes.
3. Cardiac Arrhythmias Due to β adrenergic action of
peripherally formed DA; more in patients with pre existing heart
disease.
4. Exacerbation Of
Angina Due to β adrenergic action of peripherally
formed DA; more in patients with pre existing heart
disease.
5. Alteration
In Taste Sensation
After Prolonged Therapy
1. Abnormal Movements Facial tics, grimacing, tongue thrusting, choreoathetoid movements of
limbs start appearing after a few months of use of levodopa at optimum
therapeutic dose and progress with time to include practically all patients. No
tolerance develops to this adverse effect, but dose reduction decreases severity.
Abnormal movements may become as disabling as the original disease itself—are
the most important dose-limiting side effects.
2. Behavioral
Effects Range from mild
anxiety, nightmares, etc. to
severe depression, mania, hallucinations, mental confusion or frank psychosis.
Excessive DA action in the limbic system is probably responsible
(antidopaminergic drugs are antipsychotic).
3. Fluctuation
In Motor Performance After 2–5 years of therapy, the level of
control of parkinsonian symptomatology starts showing fluctuation. ‘End of
dose’ deterioration (wearing off) which is initially gradual, develops into
rapid ‘switches’ or ‘onoff’ effect. With time ‘all or none’ response develops,
i.e. the patient is alternately well and disabled. Abnormal movements may jeopardise
even the ‘on’ phase. This is probably a reflection of progression of the
disorder: with progressive degeneration of DA neurones the ability to regulate
storage and release of DA may be largely lost: DA is then synthesized in the
striatum on a moment to moment basis resulting in rapid and unpredictable
fluctuations in motor control. Dose fractionation and more frequent
administration tends to diminish these for a time.
Cautious use is needed
in elderly; patients with ischaemic heart disease; cerebrovascular,
psychiatric, hepatic and renal disease; peptic ulcer; glaucoma, gout.
Dose: Start with 0.25 g BD
after meals, gradually increase till
adequate response is obtained. Usual dose is 2–3 g/ day.
LEVOPA, BIDOPAL
0.5 g tab.
Interactions
Pyridoxine: Abolishes therapeutic effect by enhancing peripheral
decarboxylation of levodopa; less is available to cross to the brain.
Phenothiazines, butyrophenones, metoclopramide reverse
therapeutic effect of levodopa by blocking DA receptors. The antidopaminergic
domperidone blocks levodopa induced nausea and vomiting without abolishing its
antiparkinsonian effect, because domperidone does not cross bloodbrain barrier.
Reserpine abolishes levodopa action by preventing entry of DA into synaptic
vesicles.
Nonselective MAO inhibitors: prevent degradation of peripherally
synthesized DA and NA—hypertensive crisis can occur.
Antihypertensives: postural hypotension is accentuated, reduce
their dose if levodopa is started.
Atropine, and other anticholinergic drugs have additive
antiparkinsonian action with low doses of levodopa, but retard its absorption—
more time is available for peripheral degradation —efficacy of levodopa may be
reduced.
PERIPHERAL DECARBOXYLASE INHIBITORS
Carbidopa and benserazide are extracerebral dopa decarboxylase inhibitors; they do not penetrate bloodbrain barrier
and do not inhibit conversion of levodopa to DA in the brain. Administered
along with levodopa, they increase its t½ in the periphery and make more of it
available to cross bloodbrain barrier to reach its site of action.
Benefits of the combination are—
1. The plasma t½ of
levodopa is prolonged and its dose is reduced to approximately 1/4th.
2. Systemic concentration
of DA is reduced, nausea and vomiting are not prominent— therapeutic doses of
levodopa can be attained quickly.
3. Cardiac complications
are minimized.
4. Pyridoxine reversal of
levodopa effect does not occur.
5. ‘Onoff’ effect is
minimized since cerebral DA levels are more sustained.
6. Degree of improvement
may be higher; some patients, not responding adequately to levodopa alone, also
improve.
Problems not resolved or accentuated are—
1. Involuntary
movements
2. Behavioral
abnormalities
3. Postural hypotension.
Currently, levodopa is practically always used along with a
decarboxylase inhibitor, except in patients who develop marked involuntary
movements with the combination.
Combination of levodopa with carbidopa has been given the name
‘Cocareldopa’.
BENSPAR, MADOPAR: Benserazide 25 mg + levodopa 100 mg cap.
Usual daily maintenance dose of levodopa is 0.4–0.8 g along with
75–100 mg carbidopa or 100–200 mg benserazide, given in 3–4 divided doses.
Therapy is started at a low dose and suitable preparations are chosen according
to the needs of individual patients, increasing the dose as required.
DOPAMINERGIC AGONISTS
The DA agonists can act on striatal DA receptors even in
advanced patients who have largely lost the capacity to synthesize, store and
release DA from levodopa. Moreover, they are longer acting, can exert subtype
selective activation of DA receptors involved in parkinsonism and not share the
concern expressed about levodopa of contributing to dopaminergic neuronal
damage by oxidative metabolism.
Bromocriptine
It is an ergot derivative which acts
as potent agonist on D2, but as partial agonist or antagonist on D1 receptors.
Improvement in parkinsonian symptoms occurs within ½–1 hr of an oral dose of
bromocriptine and lasts for 6–10 hours. If used alone, doses needed in parkinsonism
are high, expensive and often produce intolerable side effects—vomiting,
hallucinations, hypotension, nasal stuffiness, conjunctival injection. Marked
fall in BP with the ‘first dose’ has occurred in some patients, especially
those on antihypertensive medication.
In parkinsonism, bromocriptine is used only in late cases as a
supplement to levodopa: starting with low doses (1.25 mg once at night) and
gradually increasing as needed upto 5–10 mg thrice daily. It serves to improve
control and smoothen ‘end of dose’ and ‘onoff’ fluctuations. Dyskinesias are
less prominent with bromocriptine compared to levodopa.
PROCTINAL, SICRIPTIN, PARLODEL, 1.25, 2.5 mg tabs, ENCRIPT 2.5,
5 mg tabs.
Ropinirole and Pramipexole
These are two recently developed non-ergoline,
selective D2/D3 receptor agonists with negligible affinity for D1 and
nondopaminergic receptors. Pramipexole has relatively greater affinity for D3
receptors. Therapeutic effect as supplementary drugs to levodopa in advanced
cases of PD as well as side effect profile is similar to bromocriptine, but they
are better tolerated with fewer g.i. symptoms. Consequently dose titration for
maximum improvement can be achieved in 1–2 weeks, while the same may take
several months with bromocriptine.
Ropinirole and pramipexole
are now frequently used as monotherapy for early PD as well. Trials have found
them to afford symptom relief comparable to levodopa. Fewer cases treated with
ropinirole needed supplemental levodopa than those treated with bromocriptine.
The Parkinson Study Group and other multicentric trials have noted lower
incidence of dyskinesias and motor fluctuations among patients treated with
these drugs than those treated with levodopa. There is some indirect evidence
that use of these DA agonists may be associated with slower rate of neuronal
degeneration. Such encouraging findings indicate that the newer DA agonists are
effective alternatives to levodopa and afford longer symptom free life to PD
patients.
Ropinirole is rapidly absorbed orally, 40% plasma protein bound,
extensively metabolized, mainly by hepatic CYP1A2, to inactive metabolites, and
eliminated with a terminal t½ of 6 hrs. It is thus longer acting than levodopa,
useful in the management of motor fluctuations and reducing frequency of on off
effect.
Side effects are nausea, dizziness, hallucinations, and postural
hypotension. Episodes of day time sleep have been noted with ropinirole as well
as pramipexole. The higher incidence of hallucinations and sleepiness may
disfavour their use in the elderly.
Ropinirole has recently been approved for use in ‘restless leg
syndrome’.
Ropinirole: Starting dose is 0.25
mg TDS, titrated to a maximum of 4–8
mg TDS. Early cases generally require 1–2 mg TDS.
ROPITOR 0.25, 0.5,
1.0, 2.0 mg tabs. ROPITOR, ROPARK, ROPEWAY 0.25, 0.5, 1.0, 2.0 mg tabs.
Pramipexole: Starting dose 0.125 mg
TDS, titrate to 0.5–1.5 mg TDS.
Pergolide (bromocriptinelike)
and Piribedil (apomorphinelike) are
other DA agonists used in parkinsonism.
MAO-B INHIBITOR
Selegiline (Deprenyl)
It is a selective and irreversible MAOB
inhibitor. Two isoenzyme forms of MAO, termed MAOA and MAOB are recognized;
both are present in peripheral adrenergic structures and intestinal mucosa,
while the latter predominates in the brain and blood platelets. Unlike nonselective
MAO inhibitors, selegiline in low doses (10 mg/day) does not interfere with
peripheral metabolism of dietary amines; CA accumulation and hypertensive
reaction does not develop, while intracerebral degradation of DA is retarded.
This is responsible for the therapeutic effect in parkinsonism. Higher doses
can produce hypertensive interactions.
Selegiline alone has mild antiparkinsonian action in early
cases. Administered with levodopa, it prolongs levodopa action, attenuates
motor fluctuations and decreases ‘wearing off’ effect. As an adjuvant to
levodopa, it is beneficial in 50–70% patients and permits 20–30% reduction in
levodopa dose. However, advanced cases with ‘on-off’ effect are not improved
and the peak dose levodopa side effects such as dyskinesias, mental confusion
or hallucinations may be worsened. Moreover, clinical benefits derived from
selegiline are short lived (6–26 months).
Based on the hypothesis that oxidation of DA and/or
environmental toxins (MPTP-like) in the striatum by MAO to free radicals was
causative in parkinsonism, it was proposed that early therapy with selegiline
might delay progression of the disorder. However, no difference in the course of
the disease has been detected on follow up of selegiline treated patients in
large multicentric studies.
Adverse Effects
Postural hypotension, nausea, confusion,
accentuation of levodopa induced involuntary movements and psychosis.
Contraindicated in patients with convulsive disorders.
Selegeline interacts with pethidine causing excitement,
rigidity, hyperthermia, respiratory depression. It may also interact with
tricyclic antidepressants and selective serotonin reuptake inhibitors.
ELDEPRYL 5, 10 mg tab;
SELERIN, SELGIN 5 mg tab; Dose: 5 mg with breakfast
and with lunch, either alone (in
early cases) or with levodopa/carbidopa. Reduce by 1/4th levodopa dose after
2–3 days of adding selegiline.
COMT INHIBITORS
Two selective, potent
and reversible COMT inhibitors Entacapone
and Tolcapone have been
introduced as adjuvants to levodopa-carbidopa
for advanced PD. When peripheral decarboxylation of levodopa is blocked by
carbidopa/benserazide, it is mainly metabolized by COMT to 3Omethyldopa (see Fig. 31.2). Blockade of this pathway
by entacapone/tolcapone prolongs the t½ of levodopa and allows a larger
fraction of administered dose to cross to brain. Since COMT plays a role in the
degradation of DA in brain as well, COMT inhibitors could preserve DA formed in
the striatum and supplement the peripheral effect. However, entacapone acts only
in the periphery (probably because of short duration of action ~2 hr). For
tolcapone also, the central action is less important.
Both entacapone and
tolcapone enhance and prolong the therapeutic effect of levodopa-carbidopa in
advanced and fluctuating PD. They may be used to smoothen ‘wearing off’,
increase ‘on’ time, decrease ‘off’ time, improve activities of daily living and
allow levodopa dose to be reduced. They are not indicated in early PD cases. Entacapone: 200 mg with each dose of levodopa-carbidopa.
Tolcapone:
100–200 mg BD or TDS.
Worsening of levodopa
adverse effects such as nausea, vomiting, dyskinesia, postural hypotension,
hallucinations, etc. occurs often when a COMT inhibitor is added. However, this
can be minimised by adjustment of levodopa dose. Other prominent side effect is
diarrhoea in 10–18% patients (less with entacapone) and yellow-orange
discolouration of urine. Because of reports of acute fatal hepatitis and
rhabdomyolysis, tolcapone has been suspended in Europe and Canada, while in USA
its use is allowed only in those not responding to entacapone. Entacapone is
not hepatotoxic.
DOPAMINE FACILITATOR
Amantadine
Developed as an
antiviral drug for prophylaxis of
influenza A2, it was found serendipitiously to benefit parkinsonism.
It acts rapidly but has lower efficacy than levodopa, though higher than
anticholinergics. About 2/3rd patients derive some benefit. However, tolerance
develops over months and the efficacy is lost. Amantadine appears to act by
promoting presynaptic synthesis and release of DA in brain. Action on NMDA type
of glutamate receptors, through which the striatal dopaminergic system exerts
its influence is now considered to be more important.
Amantadine can be used in milder cases, or in short courses to
supplement levodopa for advanced cases. In the latter situation, it serves to
suppress motor fluctuations and abnormal movements. Fixed dose of 100 mg BD is
used (not titrated according to response). Effect of a single dose lasts 8–12
hours;
AMANTREL, COMANTREL
100 mg tab.
Side Effects
These are generally not serious: insomnia, dizziness,
confusion, nightmares, anticholinergic effects and rarely hallucinations. A
characteristic side effect due to local release of CAs resulting in
vasoconstriction is livedo reticularis and edema of ankles.
Side effects are accentuated when it is combined with
anticholinergics.
CENTRAL ANTICHOLINERGICS
These are drugs having a higher central : peripheral
anticholinergic action ratio than atropine, but the pharmacological profile is
similar to it. In addition, certain H1 antihistaminics have
significant central anticholinergic property. There is little to choose
clinically among these drugs, though individual preferences vary.
They act by reducing the unbalanced cholinergic activity in the
striatum of parkinsonian patients. All anticholinergics produce 10–25%
improvement in clinical features, lasting 4–8 hours after a single dose.
Generally, tremor is benefited more than rigidity; hypokinesia is affected the
least. Sialorrhoea is controlled by their peripheral action. The overall efficacy
is much lower than levodopa. However, they are cheap and produce less side
effects than levodopa. They may be used alone in mild cases and when levodopa
is contraindicated. In others, they can be combined with levodopa in an attempt
to lower its dose.
Anticholinergics are the only drugs effective in drug
(phenothiazine) induced parkinsonism.
The side effect profile is similar to atropine. Impairment of
memory and organic confusional states are more common in the elderly. The
antihistaminics are less efficacious than anticholinergics, but are better
tolerated by older patients. Their sedative action also helps. Orphenadrine has
mild euphoriant action.
Trihexyphenidyl It is the most commonly
used drug. Start with the
lowest dose in 2–3 divided portions per day and gradually increase till side
effects are tolerated.
1. Trihexyphenidyl
(benzhexol): 2–10 mg/day; PACITANE, PARBENZ 2 mg tab.
2. Procyclidine: 5–20 mg/day; KEMADRIN 2.5, 5 mg tab.
3. Biperiden: 2–10 mg/day oral,
i.m. or
i.v.: DYSKINON 2
mg tab., 5 mg/ml inj.
4. Orphenadrine: 100–300 mg/day; DISIPAL, ORPHIPAL 50 mg tab.
5. Promethazine: 25–75 mg/day; PHENERGAN 10, 25 mg tab.
