Autonomic Nervous System
| Home | | Medicinal Chemistry |Chapter: Medicinal Chemistry : Autonomic Nervous System
Autonomic nervous system (ANS) represents the unconscious regulation and controls the visceral function. It consists of afferent central connections, and autonomic efferents.
Autonomic Nervous System INTRODUCTION Autonomic nervous system (ANS) represents the unconscious regulation and controls the visceral function. It consists of afferent central connections, and autonomic efferents. The afferent nerves are the first link in the reflex of ANS, which carries nonmyelinated fibres from visceral parts to the cerebrospinal axis. Central connections refer to the integration of autonomic reflexes through hypothalamus and the nucleus solitary tract. Autonomic efferents are the principal peripheral connections that are divided into sympathetic and parasympathetic outflow. Neurotransmitter in all the pre and parasympathetic postganglion fibres is acetylcholine and in sympathetic postganglionic release is norepinephrine. ANS is composed of (1) sympathetic system and (2) parasympathetic system. Preganglionic nerves of the sympathetic system arise from the lateral gray horn of 12th thoracic segments and the first two lumbar segments of the spinal cord (thoracolumbar division). They form ganglia in the vertebral chain called paravertebral chain ganglion and supply the postganglionic fibres to effector organs. The principal neurotransmitter is adrenaline, so it is called adrenergic system. In adrenergic neurons (sympathetic postganglion), the neurotransmitter released is norepinephrine, which is also called noradrenaline. There are closely related catecholamines (CAs), that is, adrenaline and dopamine that has minor effects secreted by adrenal medulla and in limbic system basal ganglia, respectively. CAs are synthesized from amino acid phenylalanine. Tyrosine hydroxylase is the rate-limiting enzyme and its inhibition by α-methyl-p-tyrosine leads the CAs to dissipate. Other endogenous transmitter, that is, 5-HT produced by aromatic L-amino acid decarboxylase converts DOPA into dopamine and methyl dopamine, and then, it is converted by dopamine α-hydroxylase to α-methyl norepinephrine. The steps involved in the synthesis of epinephrine and norepinephrine is depicted in Figure 1.1. Noradrenaline is stored in the synaptic vesicles on the adrenergic nerve endings and released by exocytosis along with the stored adrenaline, ATP and dopamine β-hydroxylase. The CAs are metabolized by monoamine oxidase (MAO) and catechol-O-methyl transferase (COMT) in the liver and other tissues into vanillyl mandelic acid (VMA) and 3-methoxy-4-hydroxy phenyl ethylene glycol with metaephrine and normetaephrine (Fig. 1.2). They are membrane bound G-protein coupled receptors and classified as α (alpha) and β (beta) adrenoceptors. They are further classified into α1 and α2. The selective agonist for α is phenylephrine and antagonist is prazosin. α2 receptors are stimulated by clonidine selectively and antagonized by yohimbine. Elicitation of α1 receptors increases phospholipase C, D, A2, and inositol-triposphate/diacylglycerol IP3/DAG which contracts smooth muscles, genitourinary tracts, and increase the secretions of glands and in the heart, it increases the force of contraction. α1 receptor stimulation causes decrease in cyclic AMP, Ca2+ L type channels, and increases the IP3/DAG. It decrease the insulin secretion, produces platelet aggregation, decreases the release of NE as it has auto-regulation mechanism, and causes the vascular smooth muscle contraction. The β receptors are further subdivided into three subtypes and distributed in the body, that is, β1 (heart), β2 (bronchi, smooth muscles), and β3 (adipose tissue). Each has a selective agonist and antagonist. For β1 receptors, the agonist is dobutamine and antagonists are atenolol and metaprolol. Agonists for β2 are salbutamol and terbutaline and antagonist is propranolol. The pharmacology of β receptors indicate the biochemical increase of adenylcyclase, L-Type calcium channels increment through β1 causes increase in the force and rate of contraction of AV nodal conduction velocity. Β2 receptor stimulates bronchodilation through elicitation of adenylcyclase. Β3 stimulation increases adenylcyclase and causes lipolysis. Preganglionic neurons of parasympathetic system arise from III, VII, IX, and X cranial nerves and 2nd, 3rd, and 4th sacral portion of the vertebra, respectively, so its named as craniosacral outflow. Acetylcholine (ACh) is the principal neurotransmitter and also called as cholinergic neurons. ACh is released into the synaptic vesicles of effectors junction by an impulse across the neuroeffector junction. This leads to the action potential that is due to the difference in the ionic gradients of Na+ and K+ equilibrium, and in other tissues, it is mediated along with calcium ion. ACh is synthesized locally in the cholinergic nerve ending by adenosine-triphosphate (ATP) dependent system (Fig. 1.3). Choline is actively taken by the axonal membrane and acetylated with the help of ATP and co-enzyme-A by the choline acetylase. ACh is stored in the synaptic vesicles and is extruded by miniature end plate potential (MEPPS) of action potential. They are metabolized by enzymes acetyl cholinesterase and butyrocholinesterase. These convert the ACh into choline and acetate. ACh esterase comprises of an anionic site that posseses a glutamate residue and an esteric site in which histidine imidazole ring and a serine –OH group are present. Hydrolysis of Ach involves electrostatic attraction of positively charged N+ of Ach to aromatic pocket of Ach esterase and neucleophilic attack by serine –OH and activation. Hydrolysis, transfer acetyl group to serine –OH group, leaving acetylated enzyme molecule and free choline. These receptors comprise of G-Protein coupled with muscarinic and ligand gated channelled nicotinic receptors. These are selectively stimulated by muscarine. The action of muscarinic receptors may be excitatory or inhibitory. They are primarily located in the heart, blood vessels, smooth muscles, and gastrointestinal tract (GIT), sweat glands and urinary tract. There are five subtypes, that is, M1, M2, M3, M4, and M5. M1 present in the autonomic ganglia causes depolarization and also histamine release and secretes acid from gastric glands. These functions are mediated through IP3 /DAG and increase in cytostolic Ca2+ Specific antagonist is oxotremorine and agonists are pirenzipine and telenzipine. M2 is found in the sinoatrial (SA) and atrioventricular (AV) node of the heart, which decreases the rate of impulse generation and velocity of conduction, respectively. In addition, it decreases the contractility. These functions mediated through K+ channel opening decreased cAMP. M3 found in the visceral smooth muscle causes contraction, exocrine glands cause secretion, vascular endothelial release of nitiric oxide (NO) causes vasodilatation. The mechanism of the receptor is IP3/DAG elicitation and increase in Ca2+ The antagonist is hexahydrosiladifenidol and the agonist is bethanacol. M4 is similar to M2 and the M5 is similar to M1 present in CNS. These receptors are selectively agonized by nicotine and blocked by D-tubocurarine or hexamethonium. The receptors are pentameric structured and further divided into NM and NN. NM present in neuromuscular junctions cause depolarization of muscle end plate leading to contraction of skeletal muscles. The transduction mechanism is through the opening of Na+ and K+ channels. NN is present in autonomic ganglia, in adrenal medulla, and in CNS. In the ganglia level it causes depolarization and mediates the postganglionic impulse. In adrenal medulla, it stimulates the CA release through the opening of Na+ and Ca+ channels.Sympathetic System
NEUROTRANSMISSION
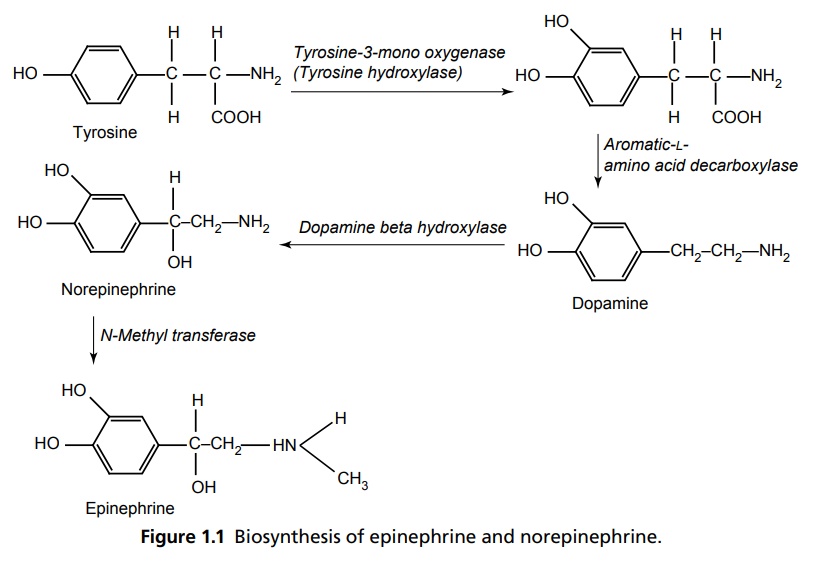
REGULATION OF CATECHOLAMINES
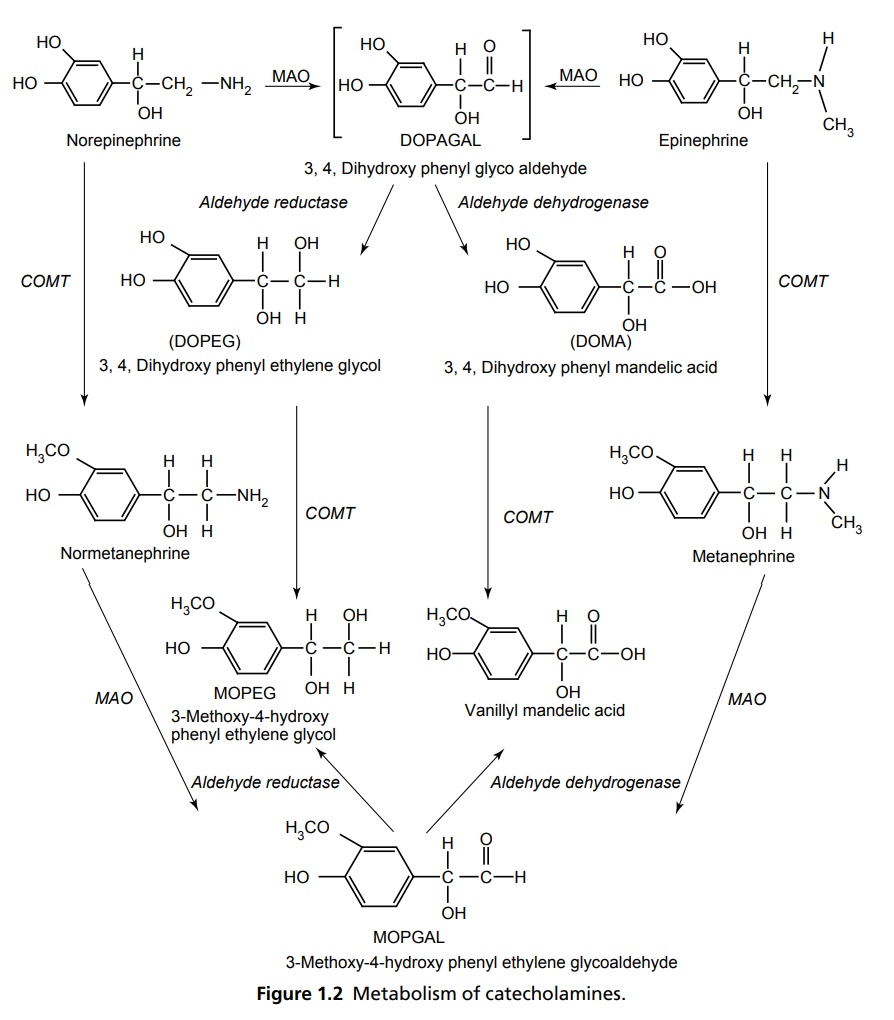
ADRENERGIC RECEPTORS
α-RECEPTORS
β-RECEPTORS
Parasympathetic System
NEUROTRANSMISSION
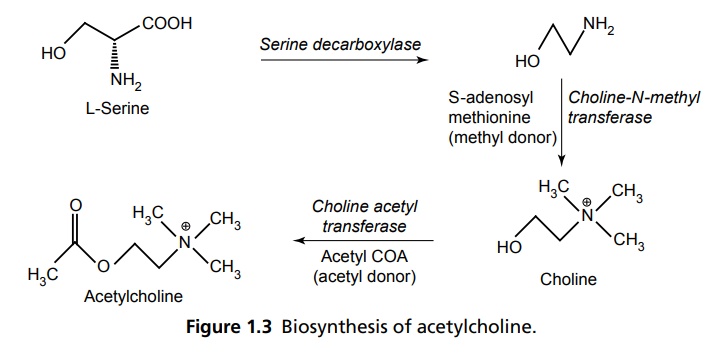
REGULATION OF ACH
CHOLINERGIC RECEPTORS
MUSCARINIC RECEPTORS
NICOTINIC RECEPTORS
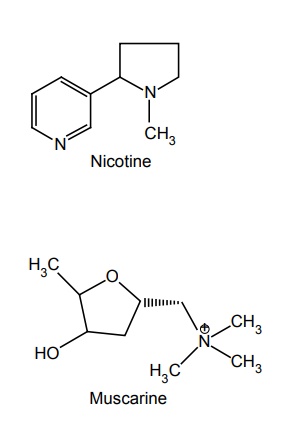
Related Topics
