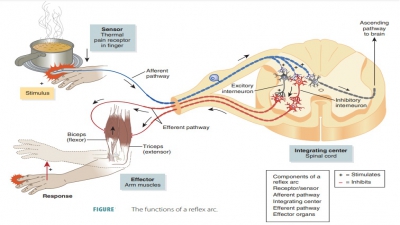
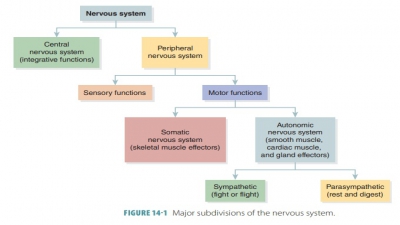
Comparison of the Somatic Nervous System and Autonomic Nervous System
| Home | | Anatomy and Physiology | | Anatomy and Physiology Health Education (APHE) |Chapter: Anatomy and Physiology for Health Professionals: Autonomic Nervous System (ANS)
Autonomic nervous system neurons are motor neurons but differ in that they contain two neurons.
Comparison of
the Somatic Nervous System and Autonomic Nervous System
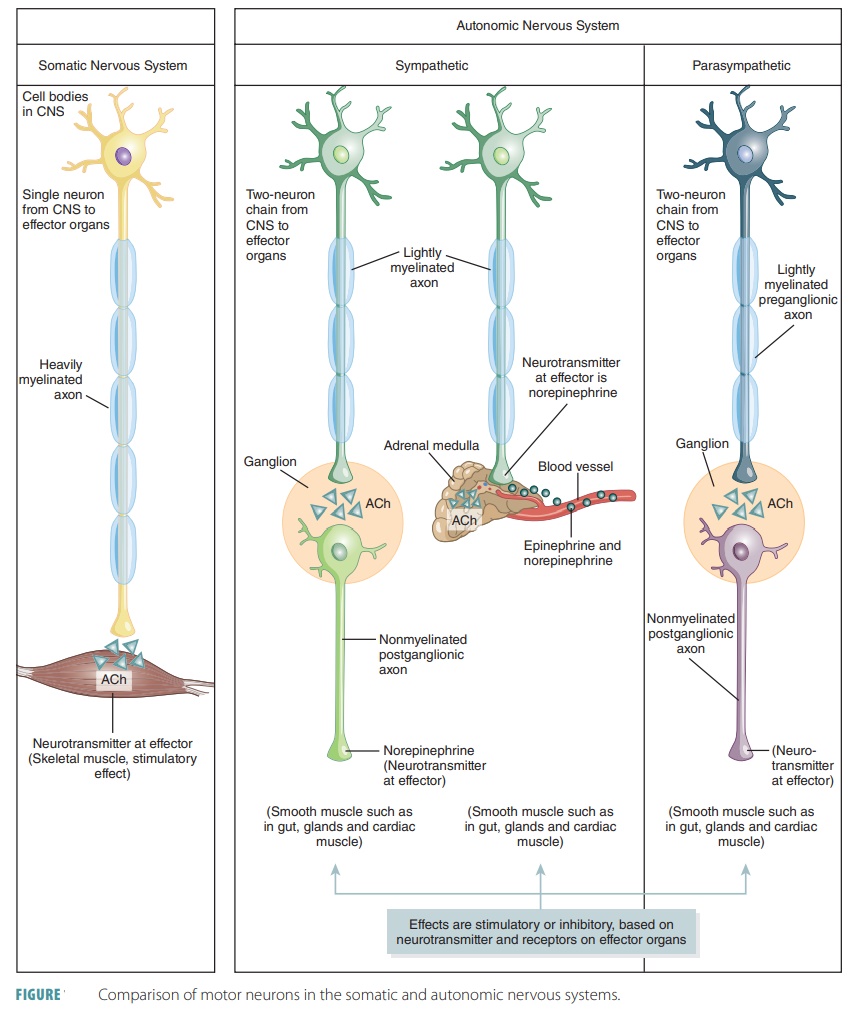
Autonomic nervous system neurons
are motor neurons but differ in that they contain two neurons (FIGURE 14-2). One
neuron’s cell body is located in the brain or spinal cord. The preganglionic axon leaves
the CNS to synapse with a second motor neuron to make a ganglionic neuron. The axon of the second neu-rons is called a postganglionic axon, which
extends to the effector organ. Preganglionic axons are thin and lightly
myelinated, whereas postganglionic axons are even thinner and unmyelinated.
Autonomic motor neurons have a
resting level of spontaneous activity even when there are no stimuli. This
determines the autonomic
tone, which is an important function
of the ANS. By keeping a rest-ing level of activity constant, an autonomic
nerve can decrease or increase its activity, allowing for better control.
Autonomic tone is important for dual innervation, but even more so when dual innerva-tion does not occur to
help balance the divisions of the body’s nervous systems. A decrease in the
autonomic tone of smooth muscle in blood vessels will cause an increase in
vessel diameter. Autonomic tone of the peripheral blood vessels would be
strongest when sympathetic simulation is increased.
Autonomic ganglia are motor ganglia and con-tain the cell
bodies of motor neurons. Conduction through the autonomic efferent chain is not
as fast as conduction in the somatic motor system. The spinal and cranial
nerves continue many pre- and postgan-glionic fibers through most of their
entire length. The autonomic ganglia are sites of synapse and informa-tion
transmission, from preganglionic to postgangli-onic neurons. The dorsal root
ganglia are only part of the sensory division of the PNS and the somatic motor
division has no ganglia at all.
Autonomic postganglionic
sympathetic fibers release norepinephrine (NE) and parasympathetic fibers
release acetylcholine (ACh). Effects are either excitatory or inhibitory,
depending on the type of receptors from the target organ. The axon terminals of
somatic neurons release ACh at the skeletal muscle fibers. This always has
excitatory effects, causing con-traction of muscle fibers. Preganglionic
sympathetic and preganglionic parasympathetic fibers release ACh. However,
postganglionic parasympathetic fibers release ACh.
Sympathetic preganglionic fibers
originate in the spinal cord. These fibers leave the spinal nerves to enter the
paravertebral ganglia. Preganglionic fibers form synapses with second neurons,
and the axons usually return to spinal nerves and visceral effectors.
Preganglionic fibers of the sympathetic nervous sys-tem that carry motor
impulses to targets in the body wall or thoracic cavity synapse in a chain
ganglion. In the parasympathetic division, preganglionic fibers arise from the
brain stem and the sacral area of the spinal cord. They lead to ganglia inside
or near the vis-cera, continuing to specific muscle or glands.
Related Topics