Specific Problems
| Home | | Pharmacovigilance |Chapter: Pharmacovigilance: Anaesthetic Adverse Drug Reactions
A systematic review has found that 9% of children experience an adverse drug reaction while in hospital.
SPECIFIC PROBLEMS
ANAESTHETIC ADVERSE DRUG REACTIONS IN CHILDREN
A
systematic review has found that 9% of children experience an adverse drug
reaction while in hospital (Impicciatore et
al., 2001). Fatal reactions reported through ADROIT data from 1964 to 2000
for chil-dren aged 16 and less identified 18 deaths out of 331 related to
anaesthetic drugs. Ten of these were from the use of inhalational anaesthetic
agents alone and thirteen were in association with propofol. Of those where
propofol was suspected, 12 were related to its use as a sedative agent. In the
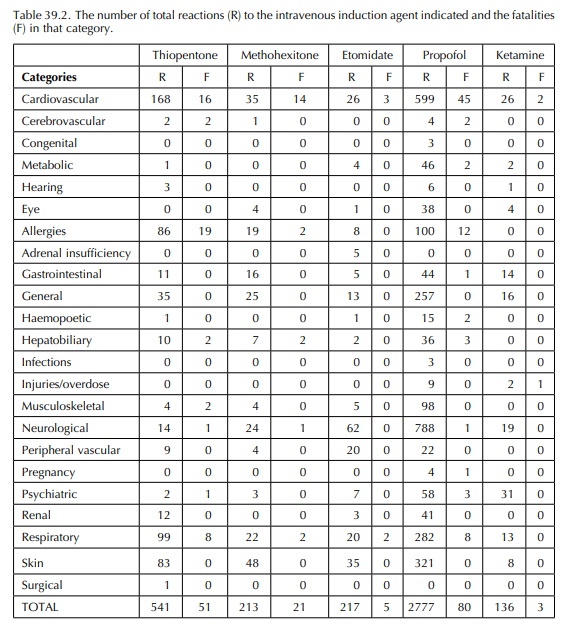
data analysis prints (Table 39.2) the reaction is peculiar to propofol but the
ages of the patients are not given. The clinical symp-toms and signs of the
reaction were first described as hyperlipidaemia, hepatomegaly, metabolic
acidosis and multiorgan failure (Parke et
al.,1992). Despite the propofol infusion syndrome being described in 1992,
further fatalities have been reported. The syndrome presents after prolonged
propofol infusion with severe metabolic acidosis unresponsive to maximum
ther-apy (Cannon, Glazier and Bauman, 2001). Acute renal failure can then
result from rhabdomyolysis, and myocardial dysfunction with bizarre, wide QRS
complexes develop without hyperkalaemia. The death of the patient is usually
from myocardial collapse with severe metabolic acidosis and multisystem organ
failure (involving renal, hepatic and cardiac systems). Thus recognition of the
context in which the risk of adverse events increases is essential in risk
prevention.
However,
despite the risk of propofol infusion syndrome being identified in 1992,
propofol infusions are still used in children. The main indication is for
short-term sedation in children requiring procedures. However, more than 1 in
10 intensivists would use propofol for prolonged sedation in paediatric
inten-sive care while monitoring for adverse events (Festa, Bowra and Schell,
2002). The maximum infusion dose that was considered dangerously high was ≥ 10 mg/kg/h for more than 72 hours.
The propo fol infusion syndrome is a rare complication first reported in
paediatric patients and believed to be due to decreased transmembrane
electrical poten-tial and alteration of electron transport across the inner mitochondrial
membrane. For the safe use of propofol infusions, there should be clear
indications and contraindications, a maximum dose rate and period of infusion
and identified minimum monitoring requirements.
CENTRAL ANTICHOLINERGIC SYNDROME
Acetylcholine
is one of the central neurotransmit-ters on which drugs used in anaesthesia
act. Anaes-thetic drugs can block cholinergic transmission to induce the
clinical picture of central anticholin-ergic syndrome, similar to atropine
intoxication. The signs are agitation, convulsions, hallucinations,
disorientation and central nervous system depres-sion such as stupor, coma and
respiratory depression (Schneck and Rupreht, 1989). Drugs that induce this
reaction include opioids, benzodiazepines, phenoth-iazines, ketamine,
etomidate, butyrophenones, propo-fol, nitrous oxide, halogenated inhalational
agents and H2-receptor blocking drugs such as cimetidine. The
anticholinesterase physostigmine is used to alleviate symptoms because it
readily crosses the blood-brain barrier thus enhancing cholinergic effects. It
does not reverse analgesia.
Related Topics
