Individual Agents
| Home | | Pharmacovigilance |Chapter: Pharmacovigilance: Anaesthetic Adverse Drug Reactions
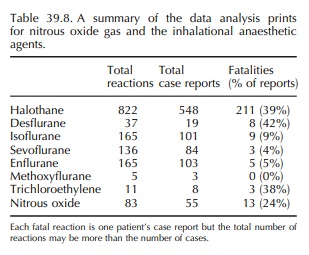
For each drug, the total number of reactions for the single drug are listed, the number of reported cases and the number of fatalities.
INDIVIDUAL AGENTS
THE INDUCTION AGENTS
The
available UK data for thiopentone, methohexi-tone, etomidate, propofol and
ketamine were obtained from voluntary reports of suspected adverse drug
reac-tions entered from yellow forms onto the Adverse Drug Reactions On-line
Information Tracking (ADROIT) database of the MHRA. They are summarised from
data analysis prints and include the reactions reported up to January 2004. In
the interpretation of the data, the causation of the event cannot be
deter-mined, comparative relationships between drugs may be misleading because
both numerator and denomina-tor data are not available, yet despite biases and
other factors, the pattern of results provides a direction that can be
exploited in the design of prospective studies.
For
each drug, the total number of reactions for the single drug are listed, the
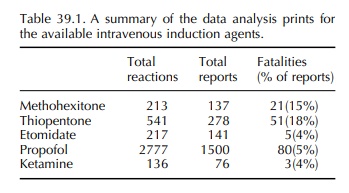
number of reported cases and the number of fatalities (Table 39.1). A multiple
drug category is listed in the data analysis prints that include the induction
agents, but it contains very small numbers of reactions so these have not been
anal-ysed here. The data contains more reactions than cases since one patient
may suffer more than one reaction; for example one patient who has an allergic
reaction may have urticaria, bronchospasm and hypotension, a total of three
reactions. The fatalities for each agent reported as a percentage of the number
of reported cases are listed in magnitude from thiopentone at 18% to etomidate
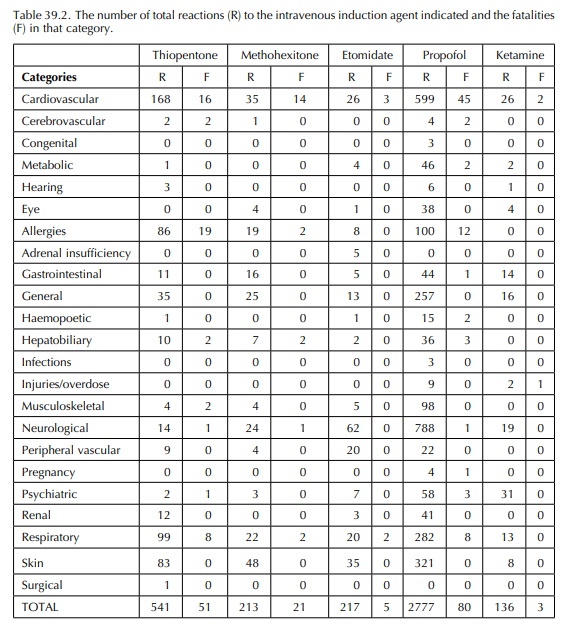
and ketamine at 4% (Table 39.1). Table 39.2 summarises the category
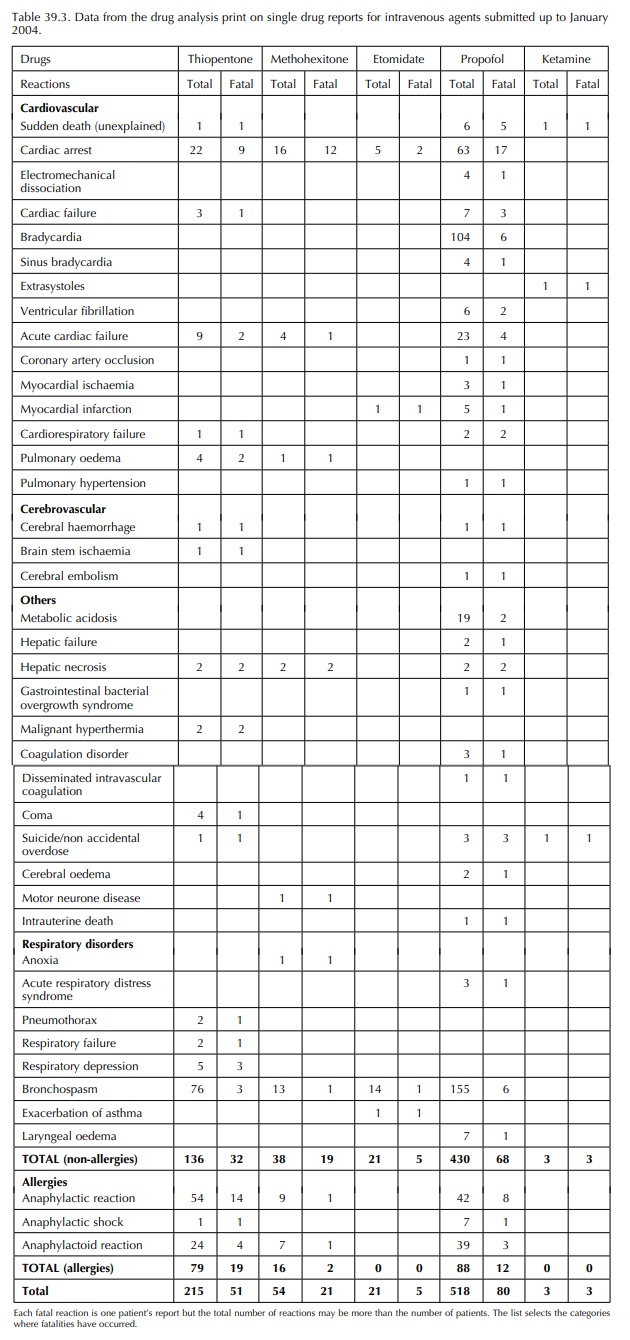
classifications for the reactions. Table 39.3 summarises the detailed diagnoses
of the fatalities and the number of reported cases in that diagnostic category.
One of the limita-tions of this data set is in the diagnostic classification,
for example ‘sinus bradycardia’ and ‘bradycardia’ are both reported separately
yet are essentially the same.
The
majority of reactions were expected, that is cardiovascular, respiratory and
allergic. Thiopentone, methohexitone and propofol are implicated in aller-gic
reactions though their incidence is not known. Althesin is no longer marketed
because of the high incidence of allergic reactions (Clarke and Watkins, 1993).
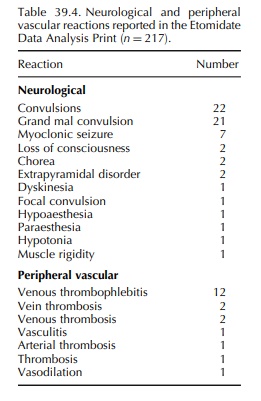
Etomidate demonstrated a profile lacking aller-gic phenomenon. However, many
more reactions reported with etomidate related to central nervous system
excitation with convulsions in the majority of reactions (Table 39.4).
Involuntary muscle move-ments can be severe, and epileptiform
electroen-cephalographic activity has been demonstrated on induction of
anaesthesia leading to the avoidance of etomidate for patients with epilepsy
(Holdcroft et al., 1976; Krieger and
Copperman, 1985). Periph-eral vascular thrombotic events of which none were
fatal were also commonly reported (Table 39.4). They may be related to the
formulation of the drug in propy-lene glycol. Part of the evidence that led to
etomidate being withdrawn from use as a sedative in an ICU setting are recorded
in Table 39.2 in the category of adrenal insufficiency. The main evidence came
from a published prospective study that demonstrated direct adrenal suppression
(Fellows et al., 1983). Even a bolus
dose can delay a rise in serum cortisol following surgery by up to 6 hours. A
prolonged infusion can cause similar effects that are not responsive to
adreno-corticotropic hormone (Ledingham et
al., 1983). A call to abandon the use of etomidate in ICUs has been made
recently (Annane, 2005), but this may not be so easy because other sedatives
also have adverse effects when used for long-term infusions.
Propofol
has a remarkable safety profile. Dose-dependent hypotension is a common
complication leading to the large number of reports of cardiovas-cular adverse
events. Clinically, these are particularly frequent in volume-depleted
patients. Hypertriglyceri-daemia and pancreatitis are uncommon complications
(Possidente et al., 1998), and
hepatobiliary fatalities are recorded in Table 39.3. For propofol, the event
that limits its use in children in the ICU is highlighted in the ‘metabolic’
column of Table 39.2 (see below for adverse drug reactions in children) and has
been called the propofol infusion syndrome. It is not confined to children and
has been identified in an adult (Perrier, Baerga-Varela and Murray, 2000). Propofol
is the only intravenous agent associated with infections (Webb et al., 1998). The main reason for this
is its formula-tion. At room temperature, propofol is an oil and insol-uble in
water. The present formulation consists of 1% or 2% (w/v) propofol, 10% soybean
oil, 2.25% glycerol and 1.2% egg phosphatide. Disodium edetate
[ethylene-diaminetetraacetic acid (EDTA)] or metabisulfite is added to retard
bacterial and fungal growth. Aller-gic complications, including bronchospasm,
have been reported with the formulation containing metabisulfite (Han, Davis
and Washington, 2001).
Fatal
reports of allergic reactions are recorded in Table 39.3. The severity of these
events is striking but the vagaries of the reporting system should be
considered. For example, in Table 39.2 in the large category of ‘skin’
manifestations there are likely to be some mild allergic reactions. The
incidence of allergic reactions to thiopentone has been estimated as 1 in 30
000 (Clarke and Watkins, 1993). Specific antibody binding tests for thiopentone
have been developed to exclude cross sensitivity to other anaesthetic agents.
There
are a small number of reported fatal reac-tions to ketamine in the data
analysis prints, and this confirms the safety of the drug in critically ill
patients. Cardiostimulatory events may cause cardio-vascular compromise as a
result of increases in cate-cholamines (Zsigmond and Kelsch, 1974). Emergence
reactions are psychomimetic, for example patients describe body detachment,
floating experiences or experience frank delirium. Long-term psychometric
reactions have been reported. Following drug use, the incidence of emergency
reactions ranges from 5% to 30% and increases with age, female sex and large
doses (Hejja and Galloon, 1975).
NEUROMUSCULAR BLOCKING DRUGS
The
21 French centres contributing to data from anaes-thetic outpatient allergy
clinics in 1990–91 reported in 1993 that an immune mechanism had been
demon-strated in 813 of 1585 patients and of these muscle relax-ants were
involved in 571 (70.3%) cases (Laxenaire, 1993). Those most often involved were
suxametho-nium (43%), vecuronium (37%), pancuronium (13%), alcuronium (8%),
atracurium (7%) and gallamine (6%). The high percentage of suxamethonium
reactions observed in this study was not explained by its rate of use because
the drug accounted for 9% of the drug market. Neither was the rate for
vecuronium easily explained, because in a previous study, adverse drug
reactions to vecuronium had been <20% and vecuronium use had not increased
dramatically. One explanation was that vecuronium had replaced suxamethonium
and thus a change in usage had occurred perhaps in a more vulnerable patient
population. Another explanation was cross-reactivity between different muscle
relaxants.
In
France from 1994 to 1996, the frequency of allergic reactions to neuromuscular
blocking drugs was highest with vecuronium followed in descend-ing order by
atracurium, suxamethonium (succinyl choline), pancuronium, rocuronium,
mivacurium and gallamine (Laxenaire, 1999). In this French group of patients,
there was a female to male ratio of 2.5, and cross-reactivity between drugs was
common (70%).
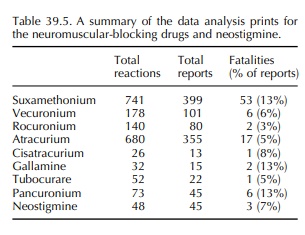
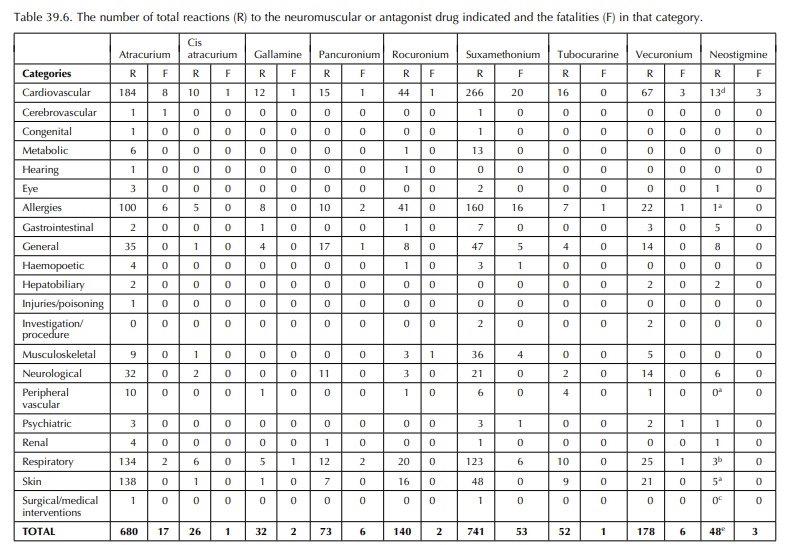
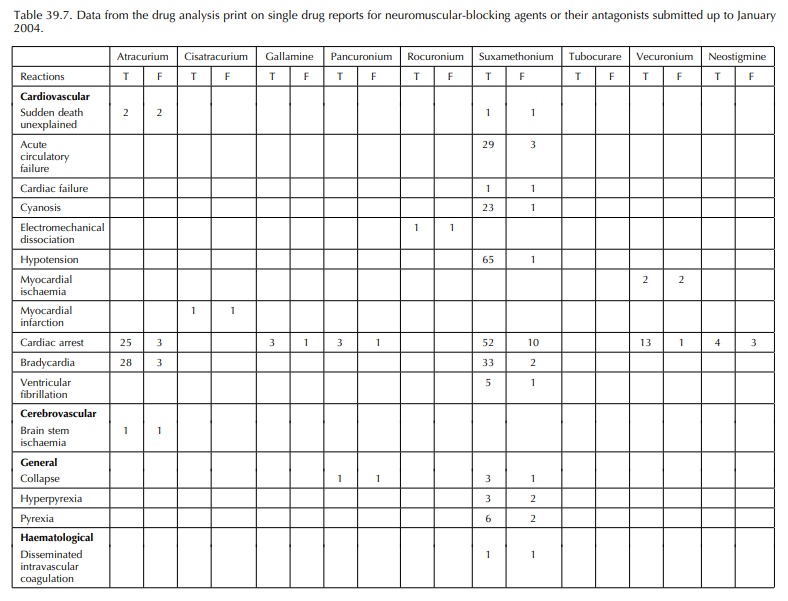
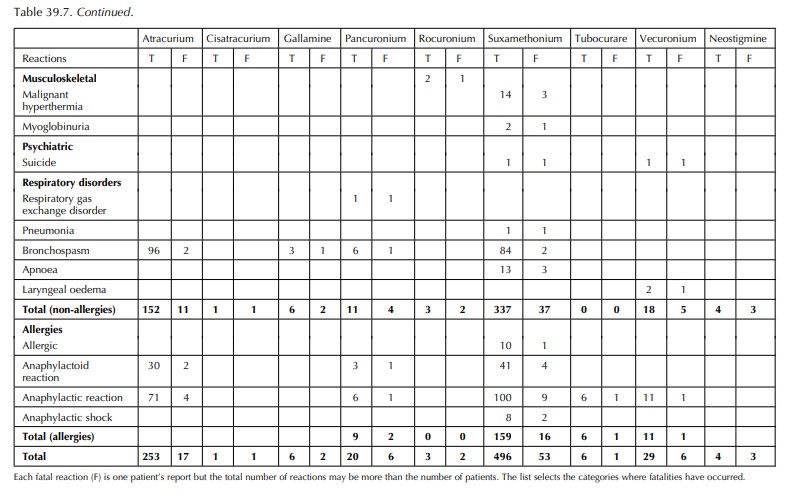
Data
analysis prints (Tables 39.5–39.7) record fatal-ities and allergies in the
atracurium, pancuronium, vecuronium and tubocurarine groups. Fatalities would
not present to out-patient allergy clinics, and so these data are useful in
identifying the potential severity of reactions, albeit not in patients
investigated for allergy. Cardiovascular and respiratory events are also
commonly reported.
INHALATIONAL AGENTS
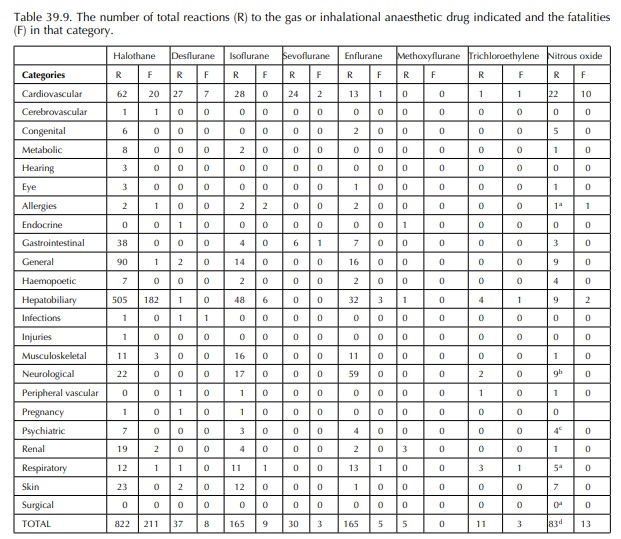
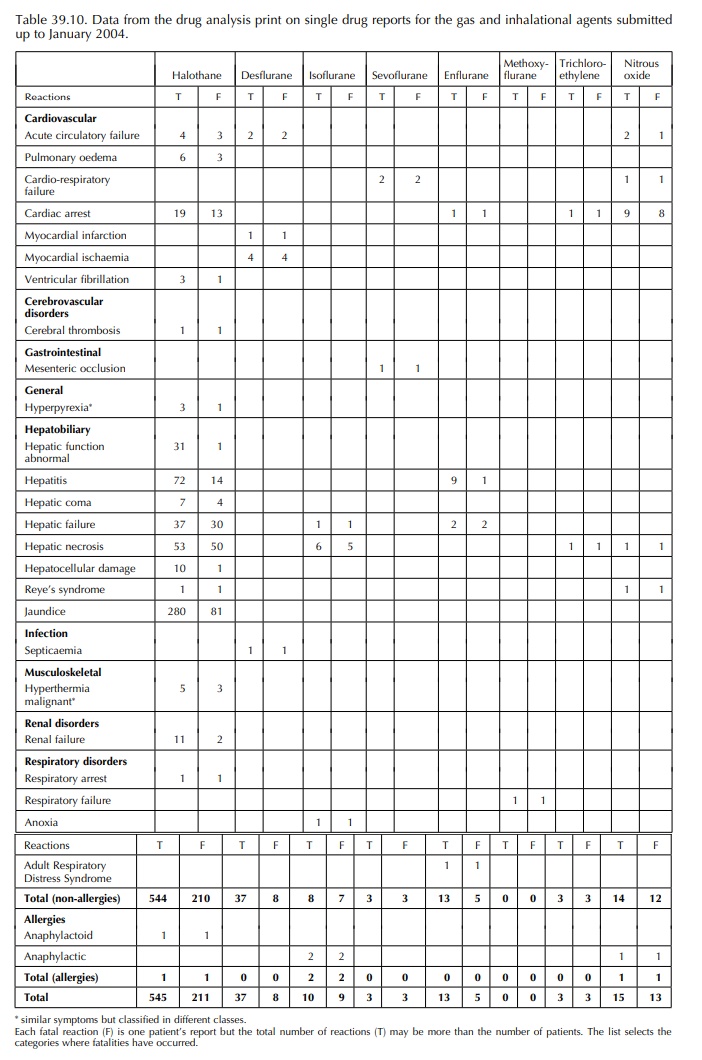
The results of the data analysis prints for halothane, methoxyflurane, trichloroethylene, isoflu-rane, sevoflurane, enflurane, desflurane and nitrous oxide have been summarised in Tables 39.8– 39.10. Table 39.9 summarises a predominance of reports relating to the hepatobiliary system, and halothane, isoflurane, desflurane, isoflurane, enflurane, methoxyflurane and trichloroethylene are all listed as single agents associated with the report. The fatalities associated with these effects are described in more detail in Table 39.10 where hepatic failure and hepatic necrosis predominate.
Halothane
is well recognised to cause hepatic damage because it is metabolised to a large
extent in the body. The other inhalational agents though are not without effect
on the liver, this activity may be in proportion to the amount metabolised, to
the particu-lar metabolic pathways, for example acetylation and types of
metabolites formed. For example, the fatal-ities associated with isoflurane
indicate that hepato-cellular damage is occurring (Reichle and Conzen, 2003).
Nephrotoxicity
has been reported for methoxy-flurane, enflurane, isoflurane and sevoflurane.
Hepatic defluorination with renal toxicity from inorganic fluoride is
considered to be the main cause of methoxyflurane effects. Renal effects
reported in the data analysis prints are small (Table 39.9) and may reflect appropriate
use of the inhalational agents and risk avoidance measures.
Long-term
exposure to clinically effective concen-trations of nitrous oxide may cause
megaloblastic bone-marrow depression and neurological symptoms. These effects
occur from an interaction with vita-min B12 resulting in selective inhibition
of methion-ine synthase, a key enzyme in methionine and folate metabolism. The
reporting of such effects in the data analysis prints is not identifiable
(Table 39.9).
LOCAL ANAESTHETICS
Table 39.11 shows the results of the UK data anal-ysis prints for the local anaesthetics lidocaine, bupi-vacaine, levobupivacaine, ropivacaine, procaine and prilocaine. For levobupivacaine, adverse drug reac-tion data collection is limited by recent licensing and hence a shorter period for reporting reactions. In addi-tion, specific reactions to local anaesthetic drugs have been reported:
• nerve toxicity with hyperbaric lidocaine
delivered intrathecally through a microcatheter during long term use;
• reduced metabolic breakdown, for example, by
drugs altering plasma cholinesterase activity or CYP450 enzymes can allow toxic
concentrations of local anaesthetic drugs to build up; and
• reduction of liver blood flow, for example,
by hypotension will decrease the hepatic clearance of amide local anaesthetics.
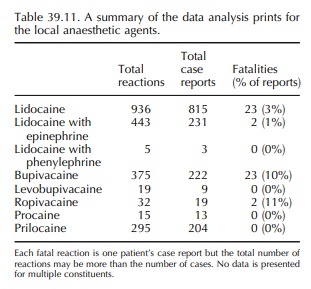
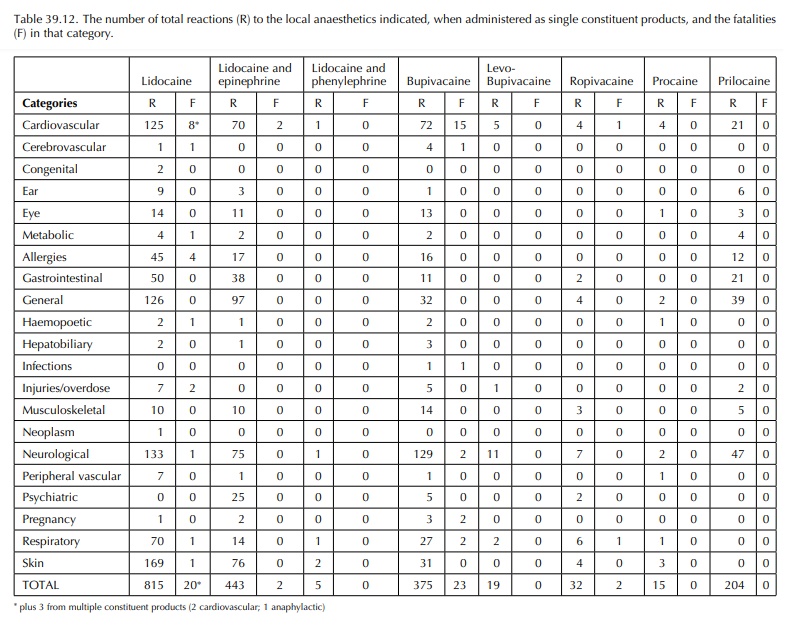
Lidocaine data (Tables 39.11–39.13) are divided into three categories because lidocaine has a different toxi-city profile when combined with a vasoconstrictor, such as epinephrine (adrenaline) or phenylephrine. In anaesthesia, lidocaine with and without epinephrine is usually available, whereas for dental procedures, the preference is for lidocaine with phenylephrine. Hence, the reported reactions may reflect the context of use and the drug delivery systems. For example, dental syringes are volume limited. Lidocaine can be readily absorbed from tissues leading to systemic absorption and toxicity. This can be prevented by constricting local blood vessels to prevent uptake into the circulation. Hence a higher total dose of lidocaine can be administered. For example, the reports of overdose with lidocaine in Tables 39.12 and 39.13 do not occur with the lidocaine and vasoconstrictor mixture. However, a lidocaine and epinephrine mixture has been associated with cardio-vascular and fatal reactions, presumably because of systemic absorption of the epinephrine. The concen-tration of epinephrine with lidocaine in the past was high, and sometimes a mixture was prepared at the bedside by a medical practitioner. Mistakes in dilu-tion used to be a risk, and nowadays, a solution pre-prepared should be used with a concentration of 1 in 200 000. What this data does not identify is the co-administration effects of volatile anaesthetic agents such as halothane with lidocaine solutions containing epinephrine. In this situation, the volatile anaesthetic agent can sensitize the myocardium and this leads to dysrrhythmias.
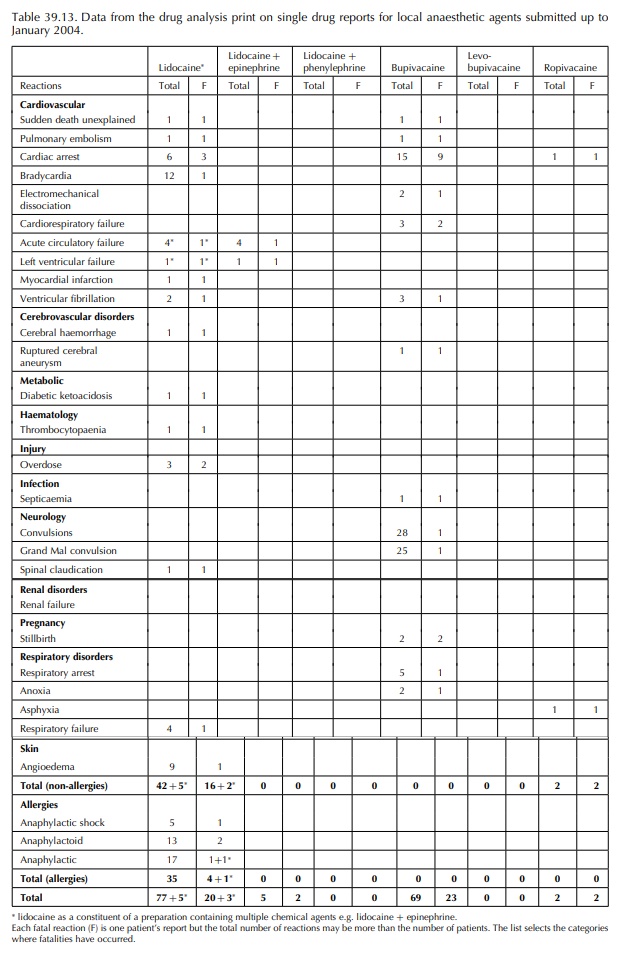
The reactions for bupivacaine also demonstrate cardiovascular events; they reflect myocardial bupi-vacaine toxicity that may be refractory to treatment (Table 39.9). Accidental intravenous injection of bupivacaine can lead to fatal cardiac arrhythmias particularly in association with a Bier’s nerve block (intravenous regional anaesthesia). The first alert of this scenario was published in 1983. Subse-quently, bupivacaine has not been recommended for intravenous regional anaesthesia. The preferred drug is prilocaine that is less toxic (Table 39.11 shows no deaths) but which in infants may induce methaemoglobinaemia.
ANALGESICS, SEDATIVES AND THEIR ANTAGONISTS
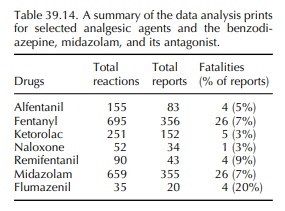
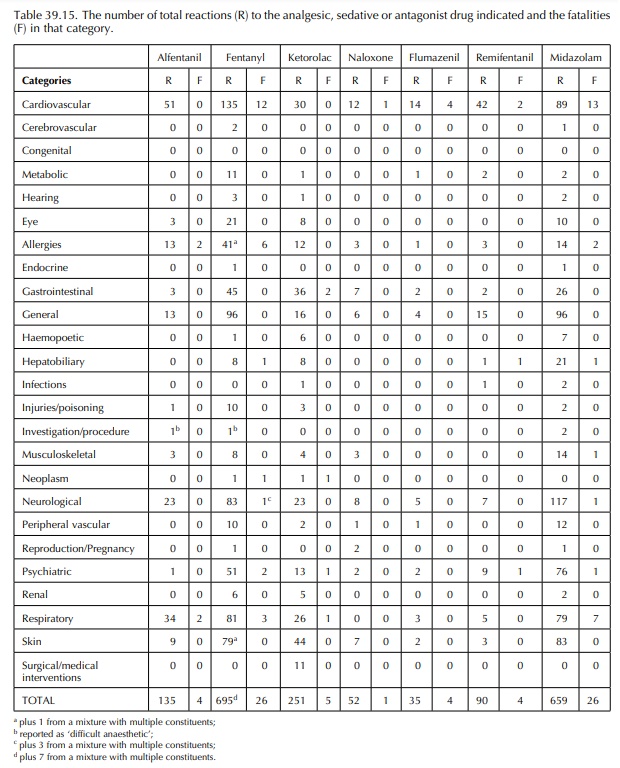
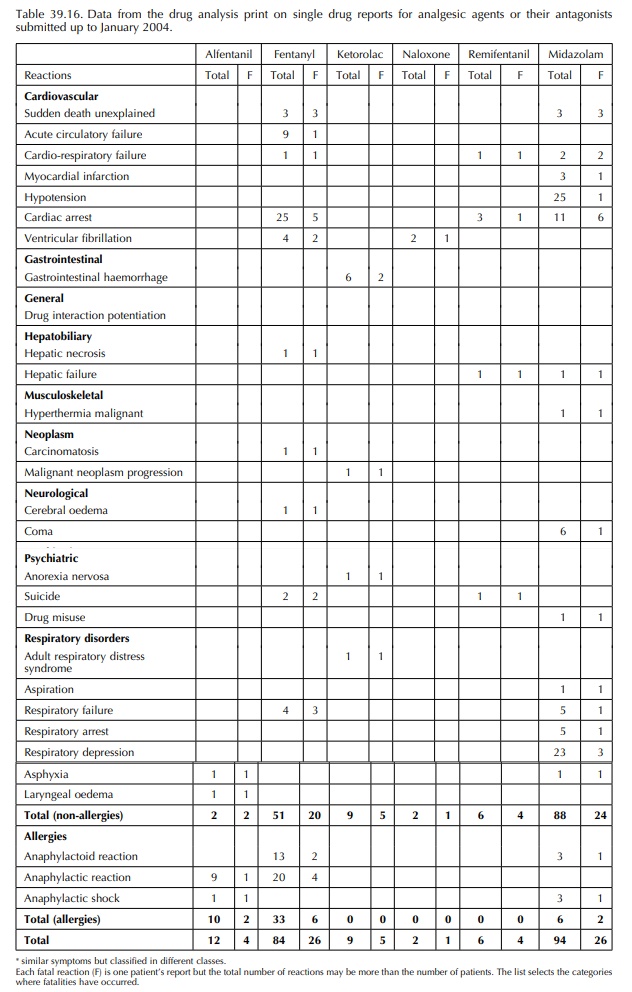
Tables
39.14, 39.15 and 39.16 show a selection of adverse effects from opioid and
non-steroidal anti-inflammatory analgesics, sedative and antagonists that are
used mainly during anaesthesia. The risks associ-ated with their long-term use
in the ICU are described in the Section ‘Introduction’. In this situation their
side effects can be more severe.
Related Topics
