Potassium Sparing Diuretics
| Home | | Pharmacology |Chapter: Essential pharmacology : Diuretics
These are either aldosterone antagonist or directly inhibit Na+ channels in DT and CD cells to indirectly conserve K+.
POTASSIUM SPARING DIURETICS
These are either aldosterone antagonist or directly inhibit Na+ channels in DT and CD cells to indirectly conserve K+.
Spironolactone (Aldosterone antagonist)
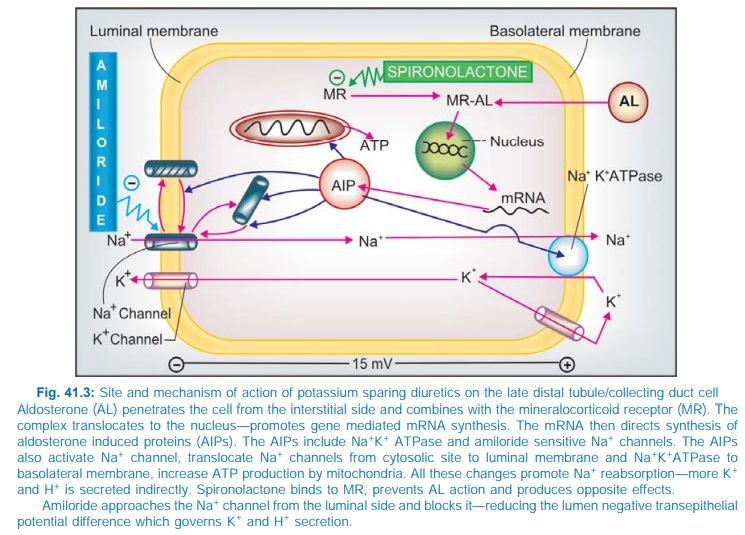
It is a steroid, chemically related to the mineralocorticoid aldosterone. Aldosterone acts on the late DT and CD cells (Fig. 41.3) by combining with an intracellular mineralocorticoid receptor → induces the formation of ‘aldosterone-induced proteins’ (AIPs) which promote Na+ reabsorption by a number of mechanisms (see legend to Fig. 41.3) and K+ secretion. Spironolactone acts from the interstitial side of the tubular cell, combines with the mineralocorticoid receptor and inhibits the formation of AIPs in a competitive manner. It has no effect on Na+ and K+ transport in the absence of aldosterone, while under normal circumstances, it increases Na+ and decreases K+ excretion.
Spironolactone is a mild saluretic because majority of Na+ has already been reabsorbed proximal to its site of action. However, it antagonises K+ loss induced by other diuretics and slightly adds to their natriuretic effect. The K+ retaining action develops over 3–4 days. It increases Ca2+ excretion by a direct action on renal tubules.
Pharmacokinetics
The oral bioavailability of spironolactone from microfine powder tablet is 75%. It is highly bound to plasma proteins and completely metabolized in liver; converted to active metabolites, the most important of which is Canrenone that is responsible for 1/2–2/3 of its action in vivo. The t½ of spironolactone is 1–2 hours, while that canrenone is ~18 hours. It undergoes some enterohepatic circulation.
Dose: 25–50 mg BD–QID; ALDACTONE 25, 100 mg tabs.
ALDACTIDE: Spironolactone 25 mg + hydroflumethiazide 25 mg tab. LACILACTONE, SPIROMIDE: Spironolactone 50 mg + furosemide 20 mg tab.
Use
Spironolactone is a weak diuretic in its own right and is used only in combination with other more efficacious diuretics.
· Edema: It is more useful in cirrhotic and nephrotic edema: aldosterone levels are generally high. It breaks the resistance to thiazide diuretics that develops due to secondary hyperaldosteronism and reestablishes the response. Thus, it is particularly employed in refractory edema.
· To counteract K+ loss due to thiazide and loop diuretics.
· Hypertension: Used only as adjuvant to thiazide to prevent hypokalaemia; has weak antihypertensive action of its own.
· CHF: As additional drug to conventional therapy in moderate to severe CHF; can retard disease progression and lower mortality.
Interactions
· Given together with K+ supplements— dangerous hyperkalaemia can occur.
· Aspirin blocks spironolactone action by inhibiting tubular secretion of canrenone.
· More pronounced hyperkalaemia can occur in patients receiving ACE inhibitors/angiotensin receptor blockers (ARBs).
· Spironolactone increases plasma digoxin concentration.
Adverse Effects
The side effects are drowsiness, confusion, abdominal upset, hirsutism, gynaecomastia, impotence and menstrual irregularities. Most serious is hyperkalaemia that may occur especially if renal function is inadequate. Acidosis is a risk, particularly in cirrhotics. Peptic ulcer may be aggravated.
Eplerenone is a recently developed more selective aldosterone antagonist, that is less likely to cause hormonal disturbances like gynaecomastia, impotence and menstrual irregularities.
Inhibitors Of Renal Epithelial Na+ Channel
Triamterene and amiloride are two nonsteroidal organic bases with identical actions. Their most important effect is to decrease K+ excretion, particularly when it is high due to large K+ intake or use of a diuretic that enhances K+ loss. This is accompanied by a small increase in Na+ excretion. The excess urinary Na+ is matched by Cl¯ and variable amounts of HCO3¯ ; urine is slightly alkalinized. The effect on urinary electrolyte pattern is superficially similar to spironolactone, but their action is independent of aldosterone.
Mechanism Of Action
The luminal membrane of late DT and CD cells expresses a distinct ‘amiloride sensitive’ or ‘renal epithelial’ Na+ channel through which Na+ enters the cell down its electrochemical gradient which is generated by Na+K+ ATPase operating at the basolateral membrane (Fig. 41.3). This Na+ entry partially depolarizes the luminal membrane creating a –15 mV transepithelial potential difference which promotes secretion of K+ into the lumen through K+ channels. Though there is no direct coupling between Na+ and K+ channels, more the delivery of Na+ to the distal nephron—greater is its entry through the Na+ channel—luminal membrane is depolarized more—driving force for K+ secretion is augmented. As such, all diuretics acting proximally (loop diuretics, thiazides, CAse inhibitors) promote K+ secretion. Amiloride and triamterene block the luminal Na+ channels— indirectly inhibit K+ excretion, while the net excess loss of Na+ is minor (most of it has already been reabsorbed).
The intercalated cells in CD possess an ATP driven H+ pump which secretes H+ ions into the lumen. This pump is facilitated by lumen negative potential. Amiloride, by reducing the lumen negative potential, decreases H+ ion secretion as well; predisposes to acidosis.
Both triamterene and amiloride are used in conjunction with thiazide type or high ceiling diuretics: prevent hypokalaemia and slightly augment the natriuretic and antihypertensive response. Risk of hyperkalaemia is the most important adverse effect of amiloride and triamterene. These drugs should not be given with K+ supplements; dangerous hyperkalaemia may develop. Hyperkalaemia is also more likely in patients receiving ACE inhibitors/ARBs, β blockers, NSAIDs and in those with renal impairment.
Both drugs elevate plasma digoxin levels.
Triamterene
It is incompletely absorbed orally, partly bound to plasma proteins, largely metabolized in liver to an active metabolite and excreted in urine. Plasma t½ is 4 hours, effect of a single dose lasts 6–8 hours.
Side Effects are infrequent: consist of nausea, dizziness, muscle cramps and rise in blood urea. Impaired glucose tolerance and photosensitivity are reported, but urate level is not increased.
Dose: 50–100 mg daily; DITIDE, triamterene 50 mg + benzthiazide 25 mg tab;
FRUSEMENE, triamterene 50 mg + furosemide 20 mg tab.
Amiloride
It is 10 times more potent than triamterene (dose 5–10 mg OD–BD). At higher doses it also inhibits Na+ reabsorption in PT, but this is clinically insignificant. It decreases Ca2+ excretion and increases urate excretion. Thus, hypercalcaemic action of thiazides is augmented but hyperuricaemic action is partly annuled. A mild antihypertensive action is also reported.
Only ¼ of an oral dose is absorbed. It is not bound to plasma proteins and not metabolized. The t½ (10–20 hours) and duration of action are longer than triamterene.
BIDURET, KSPAR: Amiloride 5 mg + hydrochlorothiazide 50 mg tab, LASIRIDE, AMIMIDE amiloride 5 mg + furosemide 40 mg tab.
Usual side effects are nausea, diarrhoea and headache.
Amiloride blocks entry of Li+ through Na+ channels in the CD cells and mitigates diabetes insipidus induced by lithium.
Given as an aerosol it affords symptomatic improvement in cystic fibrosis by increasing fluidity of respiratory secretions.
