Principles of Use of Antimicrobial Drugs
| Home | | Pharmaceutical Microbiology | | Pharmaceutical Microbiology |Chapter: Pharmaceutical Microbiology : Clinical Uses Of Antimicrobial Drugs
Drug selection should be based on knowledge of its activity against infecting microorganisms. Selected organisms may be predictably susceptible to a particular agent, and laboratory testing is therefore rarely performed.
PRINCIPLES OF USE OF ANTIMICROBIAL DRUGS
Susceptibility Of Infecting Organisms
Drug selection should be based on
knowledge of its activity against infecting microorganisms. Selected organisms
may be predictably susceptible to a particular agent, and laboratory testing is
therefore rarely performed. For example, Streptococcus pyogenes is
uniformly sensitive to penicillin. In contrast, the susceptibility of many
Gramnegative enteric bacteria is less predictable and laboratory guidance is
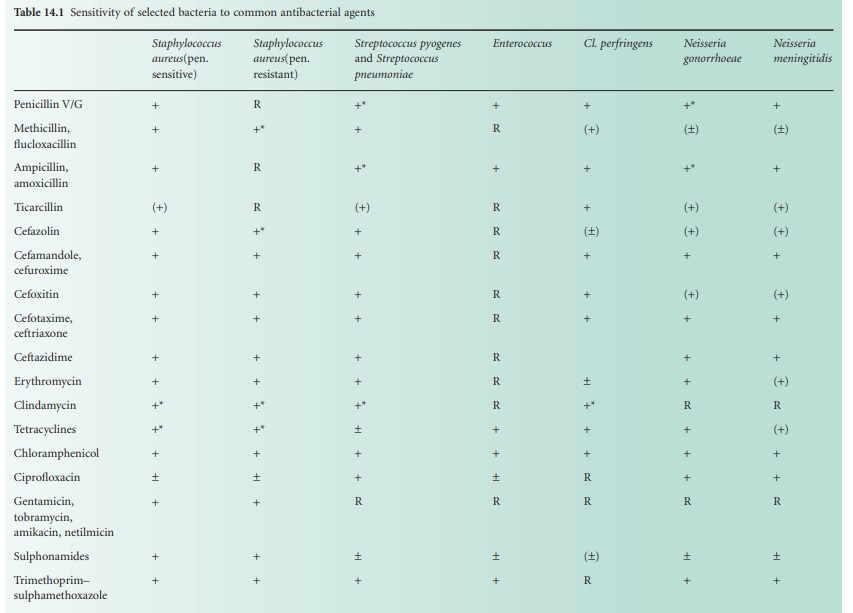
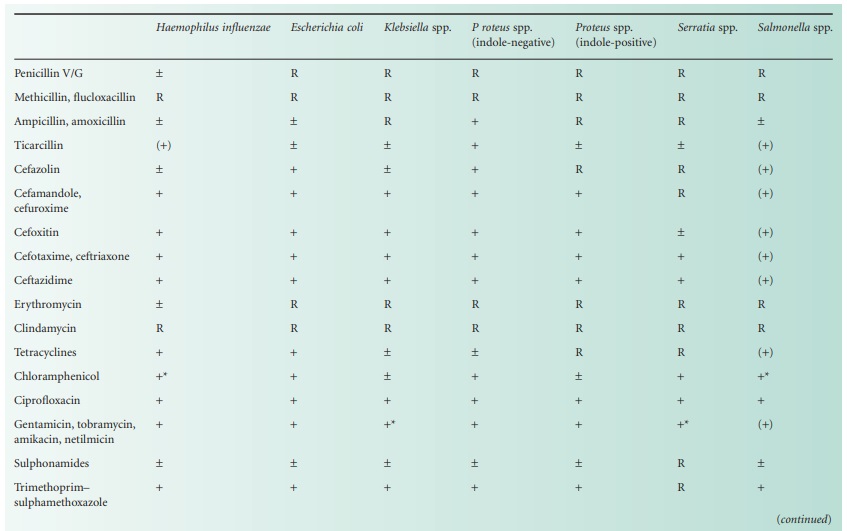
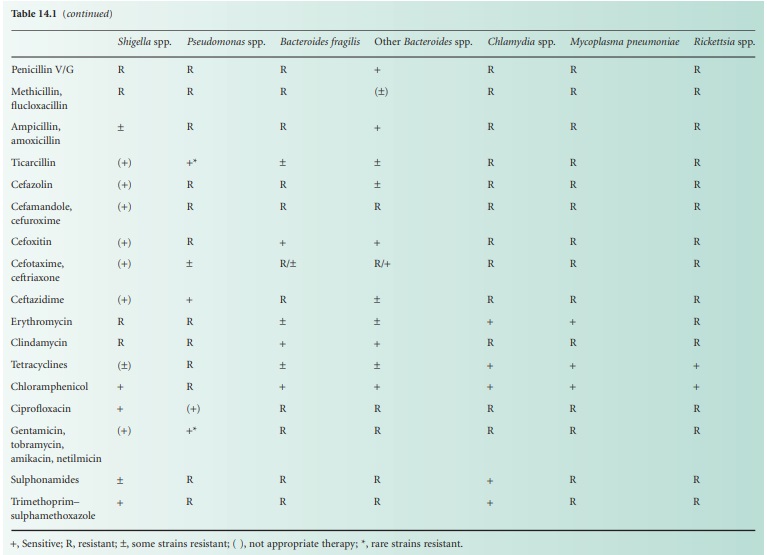
essential for safe prescribing. The susceptibility of common bacterial
pathogens and widely prescribed antibiotics is summarized in Table 14.1. It
can be seen that, although certain bacteria are susceptible in vitro to a particular agent, use of that drug
may be inappropriate, either on pharmacological grounds or because other less
toxic agents are preferred.
Host Factors
In vitro susceptibility testing does not always predict clinical outcome.
Host factors play an important part in determining outcome and this applies
particularly to circulating and tissue phagocytic activity. Infections can progress
rapidly in patients suffering from either an absolute or functional deficiency
of phagocytic cells. This applies particularly to those suffering from various
haematological malignancies, such as the acute leukaemias, where phagocyte
function is impaired both by the disease and also by the use of potent
cytotoxic drugs which destroy healthy, as well as malignant, white cells. Under
these circumstances it is essential to select agents that are bactericidal, as
bacteriostatic drugs, such as the tetracyclines or sulphonamides, rely on host
phagocytic activity to clear bacteria. Widely used bactericidal agents include
the aminoglycosides, broad-spectrum penicillins, the cephalosporins and
quinolones.
In some infections the pathogenic organisms are located intracellularly
within phagocytic cells and therefore remain relatively protected from drugs
that penetrate cells poorly, such as the penicillins and cephalosporins. In
contrast, erythromycin, rifampicin and the fluoroquinolones readily penetrate
phagocytic cells. Legionnaires’ disease is an example of an intracellular
infection and is treated with erythromycin with or without rifampicin.
Pharmacological Factors
Clinical efficacy is also dependent on achieving satisfactory drug
concentrations at the site of the infection; this is influenced by the standard
pharmacological factors of absorption, distribution, metabolism and excretion.
If an oral agent is selected, gastrointestinal absorption should be
satisfactory. However, it may be impaired by factors such as the presence of
food, drug interactions (including chelation), or impaired gastrointestinal
function either as a result of surgical resection or malabsorptive states.
Although effective, oral absorption may be inappropriate in patients who are
vomiting or have undergone recent surgery; under these circumstances a
parenteral agent will be required and has the advantage of providing rapidly
effective drug concentrations.
Antibiotic selection also varies according to the anatomical site of
infection. Lipid solubility is of importance in relation to drug distribution.
For example, the aminoglycosides are poorly lipid-soluble and although
achieving therapeutic concentrations within the extracellular fluid
compartment, penetrate the cerebrospinal fluid (CSF) poorly. Likewise the
presence of inflammation may affect drug penetration into the tissues. In the
presence of meningeal inflammation, β-lactam agents achieve satisfactory
concentrations within the CSF, but as the inflammatory response subsides drug
concentrations fall. Hence it is essential to maintain sufficient dosaging
throughout the treatment of bacterial meningitis. Other agents such as
chloramphenicol are little affected by the presence or absence of meningeal
inflammation.
Therapeutic drug concentrations within the bile duct and gallbladder are
dependent on biliary excretion. In the presence of biliary disease, such as
gallstones or chronic inflammation, the drug concentration may fail to reach
therapeutic levels. In contrast, drugs that are excreted primarily via the liver
or kidneys may require reduced dosaging in the presence of impaired renal or
hepatic function. The malfunction of excretory organs may not only risk
toxicity from drug accumulation, but will also reduce urinary concentration of
drugs excreted primarily by glomerular filtration. This applies to the
aminoglycosides and the urinary antiseptics nalidixic acid and nitrofurantoin,
where therapeutic failure of urinary tract infections may complicate severe
renal failure.
Drug Resistance
Drug resistance may be a natural or an
acquired characteristic of a microorganism. This may result from impaired cell
wall or cell envelope penetration, enzymatic inactivation, altered binding
sites or active extrusion from the cell as a result of efflux mechanisms .
Acquired drug resistance may result from mutation, adaptation or gene transfer.
Spontaneous mutations occur at low frequency, as in the case of Mycobacterium tuberculosis where a minority
population of organisms is resistant to isoniazid. In this situation the use of
isoniazid alone will eventually result in overgrowth by this subpopulation of
resistant organisms.
Genetic resistance may be chromosomal or transferable on transposons or
plasmids. Plasmid-mediated resistance has been increasingly recognized among Gram
negative enteric pathogens. By the process of conjugation , resistance plasmids
may be transferred between bacteria of the same and different species and also
different genera. Such resistance can code for multiple antibiotic resistance.
For example, the penicillins, cephalosporins, chloramphenicol and the
aminoglycosides are all subject to enzymatic inactivation, which may be plasmid
mediated. Knowledge of the local epidemiology of resistant pathogens within a
hospital, and especially within high dependency areas such as intensive care
and haemodialysis units, is invaluable in guiding appropriate drug selection.
a)
Multidrug Resistance
In recent years multidrug resistance
has increased among certain pathogens. These include Staphylococcus aureus, enterococci and M. tuberculosis. Staph. aureus resistant to meticillin
is known as meticillin-resistant Staph. aureus (MRSA). These strains are
resistant to many antibiotics and have been responsible for major epidemics worldwide,
usually in hospitals where they affect patients in high dependency units such
as intensive care units, burns units and cardiothoracic units. MRSA have the
ability to colonize staff and patients and to spread readily among them.
Several epidemic strains are currently circulating in the UK. The glycopeptides
vancomycin or teicoplanin and the oxazolidinone linezolid are the currently
recommended agents for treating patients infected with these organisms. Newer
agents such as daptomycin and tigecycline are also active against MRSA and are
increasingly used in the hospital setting; meanwhile, some strains retain
sensitivity to older agents such as tetracyclines, rifampicin and clindamycin,
and combinations of these agents are sometimes used, but only following full
analysis of microbiological sensitivities.
Another serious resistance problem is
that of drugresistant enterococci. These include Enterococcus faecalis and, in particular, E. faecium.
Resistance to the glycopeptides has again been a problem among patients in highdependency
units. Four different phenotypes are recognized (VanA, VanB, VanC and VanD).
The VanA phenotype is resistant to both glycopeptides, while the others are
sensitive to teicoplanin but demonstrate high (VanB) or intermediate (VanC)
resistance to vancomycin; VanD resistance has only recently been described and
remains uncommon. Those fully resistant to the glycopeptides are increasing in
frequency and causing great concern as they are essentially resistant to almost
all antibiotics.
Extended-spectrum β-lactamase (ESBL) producing
Gramnegative organisms are an increasing problem in hospitals, and occasionally
seen as a cause of urinary tract infection in primary care; ESBLs can hydrolyse
most cephalosporins and penicillins, limiting therapeutic options to
carbapenems or aminoglycosides. ESBLs can be chromosomally mediated (e.g. P
seudomonas spp., Citrobacter spp.) or plasmidmediated (e.g. K lebsiellaspp.),
the latter often being implicated in hospital outbreaks. Furthermore, carbapenem
resistance, via metallo β-lactamase, has been seen in outbreak strains of Pseudomonas aeruginosa and Acinetobacter baumannii; in
such situations, potentially toxic agents such as colistin are often the only
effective choice.
Tuberculosis is on the increase after decades in which the incidence had
been steadily falling. Drug-resistant strains have emerged largely among
inadequately treated or noncompliant patients. These include the homeless,
alcoholic, intravenous drug misusing, HIVpositive and immigrant populations.
Resistance patterns vary but increasingly include rifampicin and isoniazid.
Furthermore, outbreaks of multidrug-resistant tuberculosis have been
increasingly reported from a number of hospital centres in the USA and more recently
Europe, including the UK. These infections have occasionally spread to
healthcare workers and are giving rise to considerable concern.
Drug combinations
Antibiotics are generally used alone,
but may on occasion be prescribed in combination. Combining two antibiotics may
result in synergism, indifference or antagonism. In the case of synergism,
microbial inhibition is achieved at concentrations below that for each agent
alone and may prove advantageous in treating relatively insusceptible
infections such as enterococcal endocarditis, where a combination of penicillin
and gentamicin is synergistically active. Another advantage of synergistic
combinations is that it may enable the use of toxic agents where dose reductions
are possible. For example, meningitis caused by the fungus Cryptococcus neoformans responds to an abbreviated
course of amphotericin B when it is combined with 5-flucytosine, thereby
reducing the risk of toxicity from amphotericin B.
Combined drug use is occasionally
recommended to prevent resistance emerging during treatment. For example,
treatment may fail when fusidic acid is used alone to treat Staph. aureus infections, because resistant
strains develop rapidly; this is prevented by combining fusidic acid with
flucloxacillin. Likewise, tuberculosis is initially treated with a minimum of
three agents, such as rifampicin, isoniazid and pyrazinamide; again drug
resistance is prevented, which may result if either agent is used alone.
The most common reason for using combined therapy is in the treatment of
confirmed or suspected mixed infections where a single agent alone will fail to
cover all pathogenic organisms. This is the case in serious abdominal sepsis
where mixed aerobic and anaerobic infections are common and the use of
metronidazole in combination with either an aminoglycoside or a broad spectrum
cephalosporin is essential. Finally, drugs are used in combination in patients
who are seriously ill and about whom uncertainty exists concerning the microbiological
nature of their infection. This initial ‘blind therapy ’ frequently includes a
broad spectrum penicillin or cephalosporin in combination with an
aminoglycoside. The regimen should be modified in the light of subsequent microbiological
information.
Adverse Reactions
Regrettably, all chemotherapeutic agents have the potential to produce
adverse reactions with varying degrees of frequency and severity, and these
include hypersensitivity reactions and toxic effects. These may be dose related
and predictable in a patient with a history of hypersensitivity or a previous
toxic reaction to a drug or its chemical analogues. However, many adverse
events are idiosyncratic and therefore unpredictable.
Hypersensitivity reactions range in severity from fatal anaphylaxis, in
which there is widespread tissue oedema, airway obstruction and cardiovascular
collapse, to minor and reversible hypersensitivity reactions such as skin
eruptions and drug fever. Such reactions are more likely in those with a
history of hypersensitivity to the drug, and are more frequent in patients with
previous allergic diseases such as childhood eczema or asthma. It is important
to question patients closely concerning hypersensitivity reactions before
prescribing, as it precludes the use of all compounds within a class, such as
the sulphonamides or tetracyclines, while cephalosporins and carbapenems should
be used only with caution in patients who are allergic to penicillin, because
these agents are structurally related. They should be avoided entirely in those
who have had a previous severe hypersensitivity reaction to penicillin.
Drug toxicity is often dose-related and may affect a variety of organs
or tissues. For example, the aminoglycosides are both nephrotoxic and ototoxic
to varying degrees; therefore, dosaging should be individualized and the serum
assayed, especially where renal function is abnormal, to avoid toxic effects
and non-therapeutic drug concentrations. An example of dose related toxicity is
chloramphenicol-induced bone marrow suppression. Chloramphenicol interferes
with the normal maturation of bone marrow stem cells and high concentrations
may result in a steady fall in circulating red and white cells and also
platelets. This effect is generally reversible with dose reduction or drug withdrawal.
This dose-related toxic reaction of chloramphenicol should be contrasted with
idiosyncratic bone marrow toxicity which is unrelated to dose and occurs at a
much lower frequency of approximately 1:40000 and is frequently irreversible,
ending fatally. Toxic effects may also be genetically determined. For example,
peripheral neuropathy may occur in those who are slow acetylators of isoniazid,
while haemolysis occurs in those deficient in the red cell enzyme glucose 6
phosphate dehydrogenase, when treated with sulphonamides, primaquine,
quinolones or nitrofurantoin.
Superinfection
Anti-infective drugs not only affect
the invading organism undergoing treatment but also have an impact on the normal
bacterial flora, especially of the skin and mucous membranes. This may result
in microbial overgrowth of resistant organisms with subsequent superinfection.
One example is the common occurrence of oral or vaginal candidiasis in patients
treated with broad-spectrum agents such as ampicillin or tetracycline. A more
serious example is the development of pseudomembranous colitis from the
overgrowth of toxin producing strains of Clostridium difficile present
in the bowel flora following the use of clindamycin or broad-spectrum
antibiotics, though any antimicrobial can precipitate this condition. C. difficile associated diarrhoea is managed by
drug withdrawal and oral vancomycin, or oral/intravenous metronidazole.
Intravenous immunoglogbulin is occasionally used in severe cases, and rarely,
colectomy (excision of part or whole of the colon) may be necessary. Once
established, C.difficile infection is
transmissible, particularly in the hospital setting; isolation of symptomatic
patients and strict observation of hygiene practices (e.g. hand washing) are
therefore key in preventing outbreaks.
Chemoprophylaxis
An increasingly important use of antimicrobial agents is that of
infection prevention, especially in relationship to surgery. Infection remains
one of the most important complications of many surgical procedures, and the
recognition that perioperative antibiotics are effective and safe in preventing
this complication has proved a major advance in surgery. The principles that
underlie the chemoprophylactic use of antibacterials relate to the
predictability of infection for a particular surgical procedure, in terms of
its occurrence, microbial aetiology and susceptibility to antibiotics.
Therapeutic drug concentrations present at the operative site at the time of
surgery rapidly reduce the number of potentially infectious organisms and
prevent wound sepsis. If prophylaxis is delayed to the postoperative period,
then efficacy is markedly impaired. It is important that chemoprophylaxis be
limited to the perioperative period, the first dose being administered
approximately 1 hour before surgery for injectable agents; for many procedures
and operative sites, a single dose is now considered sufficient. Prolonging
chemoprophylaxis beyond this period is not cost effective and increases the
risk of adverse drug reactions and superinfection. One of the best examples of
the efficacy of surgical prophylaxis is in the area of large bowel surgery.
Before the widespread use of chemoprophylaxis, postoperative infection rates
for colectomy were often 30% or higher; these have now been reduced to around
5%.
Chemoprophylaxis has been extended to other surgical procedures where
the risk of infection may be low but its occurrence has serious consequences.
This is especially true for the implantation of prosthetic joints or heart
valves. These are major surgical procedures and although infection may be
infrequent its consequences are serious and on balance the use of
chemoprophylaxis is cost-effective.
Examples of chemoprophylaxis in the non-surgical arena include the prevention
of pneumococcal infection with penicillin V in asplenia or patients with
sicklecell disease, and the prevention of secondary cases of meningococcal
meningitis with rifampicin or ciprofloxacin among household contacts of an
index case.
Related Topics
