Vitamin D
| Home | | Biochemistry |Chapter: Biochemistry : Vitamins
The D vitamins are a group of sterols that have a hormone-like function.
VITAMIN D
The D vitamins are a
group of sterols that have a hormone-like function. The active molecule,
1,25-dihydroxycholecalciferol ([1,25-diOH-D3] calcitriol), binds to
intracellular receptor proteins. The 1,25-diOH-D3–receptor complex
interacts with DNA in the nucleus of target cells in a manner similar to that
of vitamin A (see Figure 28.20) and either selectively stimulates or represses
gene transcription. The most prominent actions of 1,25-diOH-D3 are
to regulate the plasma levels of calcium and phosphorus.
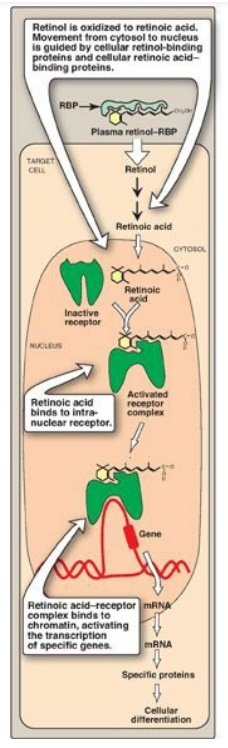
Figure 28.20 Action of the retinoids. [Note: Retinoic acid-receptor complex forms a dimer, but is shown as monomer for simplicity.] RBP = retinol-binding protein; mRNA = messenger RNA.
A. Distribution of vitamin D
1. Endogenous vitamin precursor: 7-Dehydrocholesterol, an
intermediate in cholesterol synthesis, is converted to cholecalciferol in the
dermis and epidermis of humans exposed to sunlight and transported to liver
bound to vitamin D–binding protein.
2. Diet: Ergocalciferol (vitamin D2), found in
plants, and cholecalciferol (vitamin D3), found in animal tissues,
are sources of preformed vitamin D activity (Figure 28.22). Ergocalciferol and
cholecalciferol differ chemically only in the presence of an additional double
bond and methyl group in the plant sterol. Dietary vitamin D is packaged into
chylomicrons. [Note: Preformed vitamin D is a dietary requirement only in
individuals with limited exposure to sunlight.]
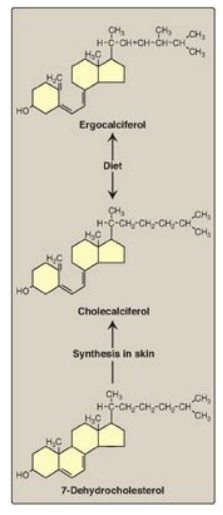
Figure 28.22 Sources of
vitamin D.
B. Metabolism of vitamin D
1. Formation of 1,25-dihydroxycholecalciferol: Vitamins D2 and D3
are not biologically active but are converted in vivo to the active form of the
D vitamin by two sequential hydroxylation reactions (Figure 28.23). The first
hydroxylation occurs at the 25 position and is catalyzed by a specific
25-hydroxylase in the liver. The product of the reaction,
25-hydroxycholecalciferol ([25-OH-D3], calcidiol), is the
predominant form of vitamin D in the plasma and the major storage form of the
vitamin. 25-OH-D3 is further hydroxylated at the 1 position by
25-hydroxycholecalciferol 1-hydroxylase found primarily in the kidney,
resulting in the formation of 1,25-diOH-D3 (calcitriol). [Note: This
1-hydroxylase, as well as the liver 25-hydroxylase, are cytochrome P450 (CYP)
proteins.]
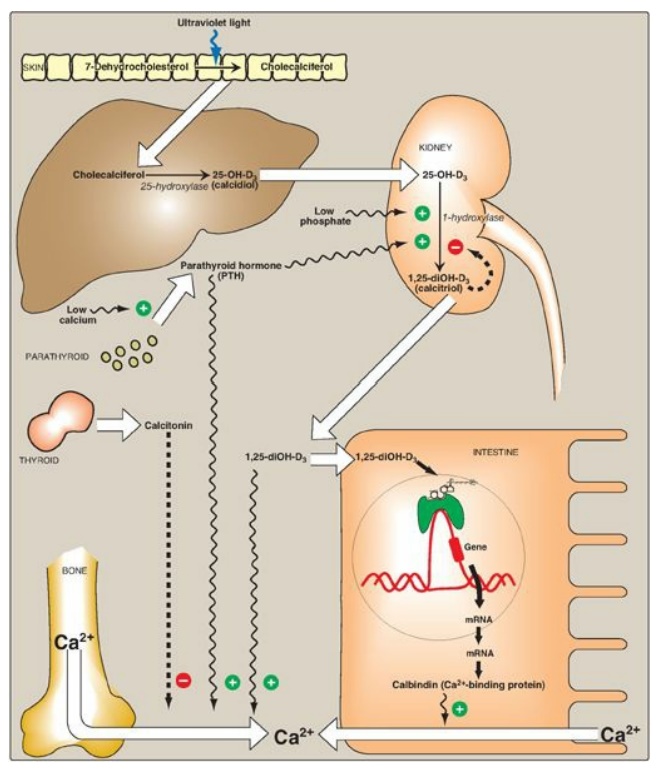
Figure 28.23 Metabolism and actions of vitamin D. [Note: Calcitonin, a thyroid hormone, decreases blood calcium by inhibiting mobilization from bone, absorption from the intestine, and reabsorption by the kidney. It opposes the actions of PTH.] mRNA = messenger RNA; 25-OH-D3 = 25-hydroxycholecalciferol; 1,25-diOH-D 3 = 1, 25-dihydroxycholecalciferol.
2. Regulation of 25-hydroxycholecalciferol 1-hydroxylase: 1,25-diOH-D3 is the most potent vitamin D metabolite. Its formation is tightly regulated by the level of plasma phosphate and calcium ions (Figure 28.24) . 25-Hydroxycholecalciferol 1-hydroxylase activity is increased directly by low plasma phosphate or indirectly by low plasma calcium, which triggers the secretion of parathyroid hormone (PTH) from the chief cells of the parathyroid gland. PTH upregulates the 1-hydroxylase. Thus, hypocalcemia caused by insufficient dietary calcium results in elevated levels of plasma 1,25-diOH-D3. [Note: 1,25-diOH-D3 inhibits synthesis of PTH, forming a negative feedback loop. It also inhibits activity of the 1-hydroxylase.]
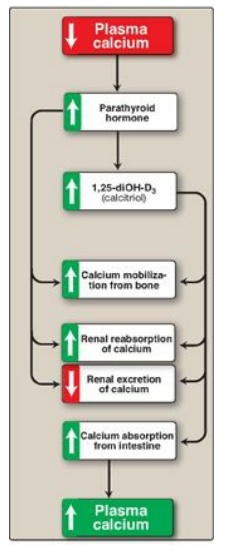
Figure 28.24 Response to low plasma calcium. 1,25-diOH-D3 = 1,25-dihydroxycholecalciferol.
C. Function of vitamin D
The overall function of
1,25-diOH-D3 is to maintain adequate plasma levels of calcium. It
performs this function by: 1) increasing uptake of calcium by the intestine, 2)
minimizing loss of calcium by the kidney by increasing reabsorption, and 3)
stimulating resorption (demineralization) of bone when blood calcium is low
(see Figure 28.23).
1. Effect of vitamin D on the intestine: 1,25-diOH-D3 stimulates
intestinal absorption of calcium. 1,25-diOH-D3 enters the intestinal cell and
binds to a cytosolic receptor. The 1,25-diOH-D3–receptor complex
then moves to the nucleus where it selectively interacts with response elements
on the DNA. As a result, calcium uptake is enhanced by an increased synthesis
of a specific calcium-binding protein, calbindin. Thus, the mechanism of action
of 1,25-diOH-D3 is typical of steroid hormones.
2. Effect of vitamin D on bone: 1,25-diOH-D3 stimulates the mobilization of calcium from bone by a process that requires protein synthesis and the presence of PTH. The result is an increase in plasma calcium and phosphate. Therefore, bone is an important reservoir of calcium that can be mobilized to maintain plasma levels. [Note: PTH and calcitriol also work together to prevent renal loss of calcium.]
D. Distribution and requirement of vitamin D
Vitamin D occurs
naturally in fatty fish, liver, and egg yolk. Milk, unless it is artificially
fortified, is not a good source of the vitamin. The RDA for individuals ages 1
to 70 years is 15 mg/day and 20 mg/day if over age 70 years. Experts disagree,
however, on the optimal level of vitamin D needed to maintain health. [Note: 1
mg = 40 international units (IUs).] Because breast milk is a poor source of
vitamin D, supplementation is recommended for breastfed babies.
E. Clinical indications
1. Nutritional rickets: Vitamin D deficiency causes a net
demineralization of bone, resulting in rickets in children and osteomalacia in adults
(Figure 28.25). Rickets is characterized by the continued formation of the
collagen matrix of bone, but incomplete mineralization results in soft, pliable
bones. In osteomalacia, demineralization of pre-existing bones increases their
susceptibility to fracture. Insufficient exposure to daylight and/or
deficiencies in vitamin D consumption occur predominantly in infants and the
elderly. Vitamin D deficiency is more common in the northern latitudes, because
less vitamin D synthesis occurs in the skin as a result of reduced exposure to
ultraviolet light.
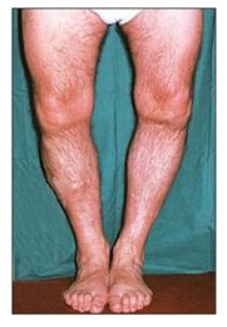
Figure 28.25 Bowed legs of middle-aged man with osteomalacia, a nutritional vitamin D deficiency that results in demineralization of the skeleton.
2. Renal osteodystrophy: Chronic kidney disease causes
decreased ability to form active vitamin D as well as increased retention of
phosphate, resulting in hyperphosphatemia and hypocalcemia. The low blood
calcium causes a rise in PTH and associated bone demineralization with release
of calcium and phosphate. Supplementation with calcitriol is an effective
therapy. However, supplementation must be accompanied by phosphate reduction
therapy to prevent further bone loss and precipitation of calcium phosphate
crystals.
3. Hypoparathyroidism: Lack of PTH causes hypocalcemia and hyperphosphatemia. These patients may be treated with calcitriol and calcium supplementation.
F. Toxicity of vitamin D
Like all fat-soluble
vitamins, vitamin D can be stored in the body and is only slowly metabolized. High
doses (100,000 IUs for weeks or months) can cause loss of appetite, nausea,
thirst, and stupor. Enhanced calcium absorption and bone resorption results in
hypercalcemia, which can lead to deposition of calcium in many organs,
particularly the arteries and kidneys. The UL is 100 mg/day (4,000 IU/day) for
individuals ages 9 years or older, with a lower level for those under age 9
years.
[Note: Toxicity is only
seen with use of supplements. Excess vitamin D produced in the skin is
converted to inactive forms.]
